|
|
|
Abstract
The use of formal and informal care for the elderly depends on many factors: income, urban-rural environment, educational attainment, family composition (singles/multi-member family), age and severity of health complications. For this analysis, a pro-rich poverty model is used based on data from the latest (8th) edition of SHARE (Survey of Health, Aging and Retirement in Europe) to examine the impact of socioeconomic inequalities among older people in the use of home care in European Union. The main results indicate that the pro-poor distribution of long-term care prevails in most of the studied countries. At the same time, health variables contribute to pro-poor inequality in the use of long-term care, mainly in informal care. When it comes to formal care, most countries have pro-poor contributions. Formal care inequalities disappeared when adjusted for need factors, while informal care inequalities remained in most countries.
Keywords: formal care; informal care; long-term care; inequity; SHARE data
JEL: I0, H4, R2
1 Introduction
Due to the uncertain future of the social sector because of the increase in the number of the elderly (over 65 years of age) and the late elderly (over 80 years), the reduced birth rate and longer life expectancy, long-term care is a leading topic in national and international policies (European Commission,  2021). Long-term care (LTC) refers to a set of activities that help a person in need to carry out their daily activities over a period of time in accordance with their physical and mental abilities (OECD, 2021). Long-term care (LTC) refers to a set of activities that help a person in need to carry out their daily activities over a period of time in accordance with their physical and mental abilities (OECD,  2005). LTC includes all those activities of care provided by another person to a beneficiary in need in formal (professional care) and informal circumstances (family members, friends, volunteers), either in organized long-term care facilities (institutions, assisted living, day centers) or in their own households (home care) for a long period of time during the day (institutions provide 24-hour care) or for several hours during the day (day care centers, home care). Although the implementation of long-term care should be based on three basic parameters proposed by the European Commission (European Commission, 2005). LTC includes all those activities of care provided by another person to a beneficiary in need in formal (professional care) and informal circumstances (family members, friends, volunteers), either in organized long-term care facilities (institutions, assisted living, day centers) or in their own households (home care) for a long period of time during the day (institutions provide 24-hour care) or for several hours during the day (day care centers, home care). Although the implementation of long-term care should be based on three basic parameters proposed by the European Commission (European Commission,  2008): universal (equal) access, high quality and sustainability of long-term care, according to the report of the European Institute for Gender Equality (EIGE, 2008): universal (equal) access, high quality and sustainability of long-term care, according to the report of the European Institute for Gender Equality (EIGE,  2020) 52% of European households cannot afford LTC. An especially important role in overcoming the financial barriers faced by users is played by the policies of the national state, that is, the share of public support. The greater the share of public support in the provision of long-term care, the greater the equality in the implementation of LTC services (Carrieri et al., 2020) 52% of European households cannot afford LTC. An especially important role in overcoming the financial barriers faced by users is played by the policies of the national state, that is, the share of public support. The greater the share of public support in the provision of long-term care, the greater the equality in the implementation of LTC services (Carrieri et al.,  2017). In addition to personal and income preferences, many other factors influence the choice and use of long-term care, the effect of which has consequences for care costs. Penning et al. ( 2017). In addition to personal and income preferences, many other factors influence the choice and use of long-term care, the effect of which has consequences for care costs. Penning et al. ( 2018) identified the key determinants of long-term care costs: features of social structure (age, gender, urban/rural environment, level of education), social and economic factors (marital status, income) and health status (chronic diseases, functional dependence). These factors are at the same time the most significant factors of the socioeconomic inequality that occurs in the provision of long-term care to the elderly population. 2018) identified the key determinants of long-term care costs: features of social structure (age, gender, urban/rural environment, level of education), social and economic factors (marital status, income) and health status (chronic diseases, functional dependence). These factors are at the same time the most significant factors of the socioeconomic inequality that occurs in the provision of long-term care to the elderly population.
Many authors (Broese Van Groenou and de Boer,  2016 2016; Saito et al.,  2018 2018) mention the connection between higher income and smaller household composition groups with the use of professional home care services, while members of smaller socioeconomically developed groups are associated with greater commitment to informal care that they provide with greater intensity. Brackley and Penning (  2009 2009) state that the use and intensity of informal home care are inversely proportional to income, i.e., wealthier individuals will use informal home care for more hours. This is refuted by Bonsang (  2009 2009) who claims that income plays a very important role in choosing a formal long-term care service, and together with a higher level of education, has a positive impact on the number of hours of care needed.
Based on previous research, our research aims to: - examine which distribution of LTC (home care) prevails in most of the countries in the European Union (EU-27)
- determine whether the use of formal care in most countries has pro-rich inequalities
- establish whether, adjusted for need factors, inequalities in home care in the EU (formal and informal care) will remain at the same level.
The research problem concerns socioeconomic inequality in the use of long-term care, while the research unit comprises the elderly person in need of long-term care. This study seeks to investigate inequality among elderly people in the use of available forms of home care (formal and informal care). The term care refers to the provision of assistance by caregivers in personal care and household chores to people who are dependent on someone else’s help (partial or total immobility, mental or physical disabilities), and does not include legal, financial or emotional support. This study will help to consider the current influencing factors, which in different socioeconomic environments affect inequalities in the use of long-term care. In addition, the latest data will provide a clear overview of the current state of the use of formal and informal care in the European Union, which is of crucial importance in planning policies for the care of elderly people. For this analysis, the model of horizontal equality based on income (pro-rich vs. pro-poor) is used, based on data from the last (8 th) edition of SHARE (Survey of Health, Ageing and Retirement in Europe) in order to examine the influence of socioeconomic inequalities among the elderly in the use of long-term care. Wagstaff, van Doorslaer and Paci (  1991 1991 ) investigated models for measuring inequalities in health and concluded that the concentration index is the best measure of socioeconomic inequalities in health. The concentration index considers the inequalities of one variable (e.g., health) in relation to another variable (e.g., income, education). The concentration index measures the level of overall health of individuals in different income classes. The main advantage is that it provides a measure of socioeconomic determinants of health inequality, one that takes into account the entire income distribution (not just the richest or the poorest). This methodology has been used in calculating horizontal equity in long-term care (Ilinca et al.,  2017 2017; Rodrigues, Ilinca and Schmidt,  2017 2017) with different age groups and when determining horizontal inequality in health care (Bago d’Uva, Jones and van Doorslaer,  2009 2009; Carrieri and Wuebker,  2013 2013; van Doorslaer, Koolman and Jones,  2004 2004). Considering that the prerequisite for the use of formal or informal care is an impaired state of health, the methodology used to calculate horizontal inequality in health care is considered relevant for defining inequality in long-term care as well. Based on research questions the following hypothesis is stated: there is a pro-poor distribution in the use of formal and informal care in European Union among elderly people.
The variables according to which the methodological part will be implemented are urban/rural environment, educational attainment, family composition (singles/ multiple family, children), income, sex, age and severity of health complications.
The structure of this study is as follows: the second part presents theoretical and empirical research on socioeconomic differences, as well as the identification of potential criteria that affect unevenly distributed long-term care (income, education, household composition, rural/urban area) among European countries. The third part presents an overview of the selected variables and the model that will be used in the research. The research results are presented in the fourth part. The discussion and conclusion of the research are contained in the fifth part of this study.
2 Theoretical and empirical research into socioeconomic differences
Wealthier people have better access to health care and better outcomes in improving their own health by using these services (van Deurzen, van Oorschot and van Ingen,  2014; Rehnberg and Fritzel, 2014; Rehnberg and Fritzel,  2016). This suggests the choice of using formal care, which was also confirmed by the research of Tenand, Bakx and van Doorslaer ( 2016). This suggests the choice of using formal care, which was also confirmed by the research of Tenand, Bakx and van Doorslaer ( 2020), which showed that the tendency to choose between professional care at home or informal care depends on income. Income and education are interrelated variables. Educated groups predominantly use formal care or a combination of formal and informal care because of their income opportunities (Kemper, 2020), which showed that the tendency to choose between professional care at home or informal care depends on income. Income and education are interrelated variables. Educated groups predominantly use formal care or a combination of formal and informal care because of their income opportunities (Kemper,  1992). Groups with lower socioeconomic status and the least education are most likely to use informal long-term care, even after accounting for differences in health status across socioeconomic groups and other resident characteristics (Bonsang, 1992). Groups with lower socioeconomic status and the least education are most likely to use informal long-term care, even after accounting for differences in health status across socioeconomic groups and other resident characteristics (Bonsang,  2009; Broese van Groenou et al., 2009; Broese van Groenou et al.,  2006). The literature finds horizontal inequality in favor of the richer in the use of paid home (professional) care in Southern Europe and horizontal equality in the use of the same services in Northern European countries (Rodrigues et al., 2006). The literature finds horizontal inequality in favor of the richer in the use of paid home (professional) care in Southern Europe and horizontal equality in the use of the same services in Northern European countries (Rodrigues et al.,  2013; Tenand, Bakx and van Doorslaer, 2013; Tenand, Bakx and van Doorslaer,  2020). Numerous organizations have called for the reduction of inequality in the health and care sector. Equal access and equal right to preventive care and the utilization of health services is one of the tasks of the World Health Organization in the “Health for All” agenda (WHO, 2020). Numerous organizations have called for the reduction of inequality in the health and care sector. Equal access and equal right to preventive care and the utilization of health services is one of the tasks of the World Health Organization in the “Health for All” agenda (WHO,  1991). Despite the efforts of international organizations, care in most countries of the European Union is determined by income, the most important parameter (Carrieri and Bilger, 1991). Despite the efforts of international organizations, care in most countries of the European Union is determined by income, the most important parameter (Carrieri and Bilger,  2013). Van Doorslaer, Koolman and Jones ( 2013). Van Doorslaer, Koolman and Jones ( 2004) found that there are significant disparities in health and long-term care in favor of the richer in all countries, but especially in Portugal, the United Kingdom, and Denmark. Low inequalities, on the other hand, were found in the Netherlands, Germany, Italy, Belgium, Spain, Austria, and Ireland. The latest studies indicate an increase in social equality compared to previous years, and the visibility of these inequalities is manifested at the international and national level (Eurofound, 2004) found that there are significant disparities in health and long-term care in favor of the richer in all countries, but especially in Portugal, the United Kingdom, and Denmark. Low inequalities, on the other hand, were found in the Netherlands, Germany, Italy, Belgium, Spain, Austria, and Ireland. The latest studies indicate an increase in social equality compared to previous years, and the visibility of these inequalities is manifested at the international and national level (Eurofound,  2017). Although equality in the implementation of long-term care is guaranteed by numerous national and international rights, there is still visible heterogeneity in the implementation of these services. Different local development is a potential source of inequality in the use of LTC. On the other hand, the share of informal care in the countries of Southern, Central and Eastern Europe is remarkably similar (Barbieri and Ghibelli, 2017). Although equality in the implementation of long-term care is guaranteed by numerous national and international rights, there is still visible heterogeneity in the implementation of these services. Different local development is a potential source of inequality in the use of LTC. On the other hand, the share of informal care in the countries of Southern, Central and Eastern Europe is remarkably similar (Barbieri and Ghibelli,  2018). The reason for this should also be found in established family relationships, where the countries of Southern and Eastern Europe traditionally nurture large families and societal norms that mandate the care of elderly parents. Nordic and Continental European countries represent smaller nuclear families, often dislocated from elderly parents, and according to social understanding, they have no obligation to sacrifice their own career or family to help an elderly father or mother. Better developed environments have better systems and opportunities to use long-term care, as evidenced by the term “postal code lottery” (Rodrigues, Ilinca and Schmidt, 2018). The reason for this should also be found in established family relationships, where the countries of Southern and Eastern Europe traditionally nurture large families and societal norms that mandate the care of elderly parents. Nordic and Continental European countries represent smaller nuclear families, often dislocated from elderly parents, and according to social understanding, they have no obligation to sacrifice their own career or family to help an elderly father or mother. Better developed environments have better systems and opportunities to use long-term care, as evidenced by the term “postal code lottery” (Rodrigues, Ilinca and Schmidt,  2017), which is the result of infrastructural facilities adopted for long-term care in local municipality and organized domestic assistance programs in the house care. The elderly in more urban areas most often use a formal version of care, because of the greater availability of this form, whether it is the provision of care at home or in an institution (Lera, Pascual-Sáez and Cantarero-Prieto, 2017), which is the result of infrastructural facilities adopted for long-term care in local municipality and organized domestic assistance programs in the house care. The elderly in more urban areas most often use a formal version of care, because of the greater availability of this form, whether it is the provision of care at home or in an institution (Lera, Pascual-Sáez and Cantarero-Prieto,  2021). The use of different types of services is not the same in all regions, so it can be concluded that better developed environments have developed a greater number of available services for the provision of long-term care (Fernandez and Forder, 2021). The use of different types of services is not the same in all regions, so it can be concluded that better developed environments have developed a greater number of available services for the provision of long-term care (Fernandez and Forder,  2015). Of course, this also depends on the geographical positioning of a local self-government unit and its dependence on the central part of the country. In rural areas, 80% of people with lower incomes and major illnesses (dementia) use informal services (Chuakhamfoo et al., 2015). Of course, this also depends on the geographical positioning of a local self-government unit and its dependence on the central part of the country. In rural areas, 80% of people with lower incomes and major illnesses (dementia) use informal services (Chuakhamfoo et al.,  2020). The reason for this is the lower disposable income of users and limited access to information about the possibilities of using long-term care (Albertini and Pavolini, 2020). The reason for this is the lower disposable income of users and limited access to information about the possibilities of using long-term care (Albertini and Pavolini,  2017; Ilinca et al., 2017; Ilinca et al.,  2017). Living in a multi-member family provides the opportunity for one of the members to become a provider of informal care and according to Rodrigues et al. ( 2017). Living in a multi-member family provides the opportunity for one of the members to become a provider of informal care and according to Rodrigues et al. ( 2013) wives and children are the most important source of informal care. Informal care is the most common choice of care among lower income families because their caregivers have lower opportunity costs when losing their job (Sarasa and Billingsley, 2013) wives and children are the most important source of informal care. Informal care is the most common choice of care among lower income families because their caregivers have lower opportunity costs when losing their job (Sarasa and Billingsley,  2008). Also, family members often act as advocates when choosing long-term care services (Rodrigues, Ilinca and Schmidt, 2008). Also, family members often act as advocates when choosing long-term care services (Rodrigues, Ilinca and Schmidt,  2017) especially in rural areas and in households with lower incomes that are initially disadvantaged due to limited access to information and types of services. 2017) especially in rural areas and in households with lower incomes that are initially disadvantaged due to limited access to information and types of services.
Depending on the national plan and program, many countries in Europe subsidize the resort to home care as an adequate substitution for the institutional type of accommodation. The Nordic countries have successfully implemented the deinstitutionalization process and emphasized the importance of using home care. On the other hand, in many European countries, the informal form of care takes precedence over the formal due to the insufficient development of the system.
3 Data and methods
In this study we are exploring socioeconomic inequalities in utilization of formal and informal long-term care (LTC) in the elderly population (over 65 years). To this end we employed the concentration index (CI), a synthetic measure of inequality in healthcare related to socioeconomic status (SES) (Wagstaff, van Doorslaer and Paci,  1991; Wagstaff and van Doorslaer, 1991; Wagstaff and van Doorslaer,  2000) which measures income inequality in the use of health services and is written as follows: 2000) which measures income inequality in the use of health services and is written as follows: 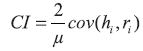 | (1) |
 2009): 2009): | CCI = 4 * μ * CI = 8cov(hi, ri) | (2)
|
In order to obtain more informative results, a decomposition of CI into contributing factors was implemented. Each one of these factors contributes to the overall CI, with some factors contributing to the pro-rich direction, while others pull the CI in the opposite direction, i.e., pro-poor. The contributions of individual factors are modeled by considering both the effect that the given factor has on the level of utilization, and also the distribution of the said factor in relation to SES. The former is called elasticity, measuring how sensitive the LTC is to variation in the said factor. The latter is called a partial concentration index, measuring how equal the distribution of the said factor is with respect to SES. The factor contributions are proportional to the product of elasticity and partial CI, meaning that factors with large elasticity but very small partial CI will have small contributions, as well as factors with very small elasticity and large partial CI, so only factors in which both elasticity and partial CI are pronounced will significantly contribute to overall CI. Also, the signs of elasticity and partial CI will determine the sign of the contribution, with same signs (++ or – –) giving a positive, i.e., pro-rich contribution, and different signs (+– or –+) producing a negative (pro-poor) contribution.
Another question not answered by previously described analyses is: to what extent is LTC driven by dependency and need for care? To this end we employ a method called analysis of equity, in which horizontal inequity index (HI) is a measure of inequality. Empirical research on equity in health care utilization examines horizontal equity, defined as equal treatment for equal need, independent of characteristics such as SES, for which differences in health care are considered unacceptable. In practice, treatment is measured by health care utilization and need by health indicators and demographic characteristics. Horizontal inequity is determined by comparing the deviation of the actual distribution of health care from that which would result if utilization were determined by need alone. In other words, equity analysis is based on the principle that individuals with the same level of need for care should receive the same level of care regardless of other potential factors, so positive or negative values signal unequal treatment of equal needs. We calculate the HI using the indirect standardization method (van de Poel, van Doorslaer and O’Donnell,  2012 2012), where HI is obtained as the difference between overall CI and the contributions of all the need factors used in the study, leaving the contributions of non-need factors.
The analyses were performed using R: A Language and Environment for Statistical Computing together with a set of open-source R packages. CI calculation and decomposition was performed with the help of rineq package which is based on decomp package. 1
We used specific methodological documentation based on Bergmann and Börsch-Supan (  2021 2021). The analysis is based on microdata from the eighth wave of the Survey of Health, Ageing and Retirement in Europe (SHARE), collected during 2019/2020 in 26 European countries. Israel was part of the SHARE survey but was not included in this sample (not an EU member). The sample consists of people aged 65 or older at the time of the survey. Where possible, imputed values prepared by SHARE were used for variables with many missing values. Of the initial 46,733 subjects, due to these restrictions and missing values, 31,340 individuals were left in the study. Of these 15,393 excluded individuals, 12,327 were younger than 65 years, the remaining 824 were individuals from Israel, and 2,241 were due to missing values. Most missing values were recorded for the variable Area (1505), with the Czech Republic having the most missing values in absolute numbers (174 or 7.7%) and Slovakia having the most missing values in relative numbers (48 or 10.6%). The remaining 736 missing values were recorded for the Formal Care variable (520, most for Belgium: 56 or 3.9%), Informal Care (156, most for Italy: 21 or 1.3%), and the three Health variables, all of which had fewer than 10 individuals with missing values. There were also some negative values recorded in the responses for the health variables that were excluded, 50 in total. Formal LTC use was measured by a synthetic indicator of use in the last 12 months, which captures professional support including personal care, domestic tasks, other activities and meals-on-wheels. Informal LTC use was measured by the synthetic use indicator in the last 12 months, which includes non-professional support from outside the household as well as inside. Socioeconomic status (SES) was proxied by equivalized net household income, using square root scale and adjusted for purchasing power parity of each country, according to the formula:
equivalized income = household income / sqrt(# people in household)
* exchange rate / ppp rate | (3) |
4 Results
Descriptive statistics of all dependent and independent variables with sample sizes are presented in table 1, broken down for each analyzed country.
Table 1Descriptive statistic of all dependent and independent variables DISPLAY Table
Dependent variables are formal and informal care use. Formal care use ranges in proportion from the lowest, 2.6% in Romania, to 28.1% in Belgium, while informal care use is lowest in Malta 10.7% and highest in the Czech Republic 40.6%. High use of formal care was also recorded in Cyprus and Spain, followed by France, the Netherlands, Austria, and Germany (15.3%). Interestingly, it was lower in countries such as Denmark, Switzerland and Finland. Formal care was lowest in Eastern European, Southeastern European and Baltic countries. Informal care was very high in Austria (38.9%), Estonia and Denmark, followed by Finland, Croatia, Germany, Romania, Belgium, Bulgaria and France (28.4%). It was below 20% in Malta (10.7%), Slovakia, Poland, Italy, Luxembourg and Spain (19.2%). The remaining countries had scores between 20.8% and 26.1%.
Independent variables (factors) are separated into need factors: SP health, ADL, Chronic, Age, Gender; and non-need factors: Area, Married, Children, Income, Education. SP (self-perceived) health is a variable scored on a scale from 1 – Excellent to 5 – Poor, and because it assumes 5 different values with an approximate symmetrical distribution, it is used in the analyses as a continuous variable with numeric values. Poorest scores were recorded for Latvia (4.11), Estonia, Lithuania, Romania, Poland, Croatia, Bulgaria and Hungary (3.54), while the best scores were seen in Denmark (2.68), Switzerland, Sweden and Netherlands (2.96). All other countries had scores between 3 and 3.5.
Most of the elderly in the analyzed countries declare they are of average health status, with the best self-perceived score in Denmark and the worst in Latvia. ADL (activities of daily living limitations) is also treated as a continuous variable, along with Chronic (number of chronic diseases). The worst ADL scores were found for Spain (0.54), Lithuania, Romania, Cyprus, Poland, and Estonia (0.40); the best scores were found for Switzerland (0.11), the Netherlands, Malta, Denmark, Sweden, and Finland (0.18); and the remaining countries ranged from 0.21 to 0.36. The most chronic diseases were reported for Poland (2.83), Luxembourg, Cyprus, Lithuania, Croatia, Czech Republic, Greece, Spain, and Finland (2.34), the least for Switzerland (1.53), Slovakia, the Netherlands, Malta, Sweden, Denmark, Italy, and Romania (1.94), while the remaining countries ranged from 2.04 to 2.32.
Age is a continuous variable measuring age of respondents, and the mean values were in the range from 71.7 for Slovakia to 77.1 for Spain. Gender is a dichotomous categorical variable, indicating if an individual is of a female gender. There were the fewest female respondents in Germany (50.9%) and the most in Latvia (66%). The highest average age is detected in Spain and regarding gender, all EU countries have dominant share of women in the population of elderly people. Area is a dichotomous categorical variable with a positive category defining rural area, where an original variable with five categories was grouped into two categories, with first category encompassing all city and town areas, and second category defining only rural areas. The countries with the fewest rural areas were Sweden (16.7%), Greece, Belgium, the Netherlands, Spain, Cyprus, Denmark, and Malta (24.3%), while the countries with the most rural areas were Romania (75%), Slovakia, Switzerland, Poland, Bulgaria, France, Finland, and Luxembourg (45.1%). The variable “Married” is a dichotomous categorical variable with the first category including original categories “Never married”, “Divorced”, “Widowed”, and second including “Married, living with spouse”, “Registered partnership”, “Married, not living with spouse”. The fewest respondents in the married category were in Latvia (50.6%) and the most were recorded in Netherlands (78.7%).
Children is a continuous variable measuring number of children, with the lowest average number of children recorded for Hungary (1.79) and the highest for Cyprus (2.55). Income is a continuous measure of SES. The countries with the lowest income of respondents were Bulgaria (653), Romania, Hungary, Estonia, Croatia, Lithuania and Latvia (1,098), while the highest incomes were recorded for Cyprus (6,565), Switzerland (3,837), Luxembourg, Finland, Denmark, Austria, France and Germany (2,062). It is interesting to note that Cyprus has the highest income, while Switzerland, in second place, has a much lower mean. The income distributions are very skewed, with most values at the lower end of the range. Comparing the income distributions for these two countries, we see that Cyprus has many more values at the high end of the range than Switzerland, implying that there are more wealthy individuals among respondents in Cyprus. Looking at another measure of central tendency, the median, which marks the point at which 50% of respondents are below and 50% are above this point, both countries had almost the same median value around the year 2000. The median income value for Cyprus was so high because many more respondents had high and very high incomes. Also, this variable is equivalized income, so the original income was corrected for PPP. The PPP ratio between Switzerland and Cyprus was about 2, so this variable was also inflated for Cyprus. The likely reason for this phenomenon is that Cyprus is a popular immigration destination for wealthy retirees from other countries, especially from the United Kingdom, so a large proportion of the respondents consists of these immigrants, whose incomes are much higher than those of native-born Cypriots.
Education measures the overall number of years of the individual’s formal education. The countries with the lowest number of years of education were Italy (8.24), Spain, Cyprus, Romania, Greece, Austria, and Malta (9.26); the highest values were recorded for Denmark (13.35), Germany, Belgium, the Czech Republic, the Netherlands, and Sweden (12.02).
It is interesting to compare some countries based on these values. For example, seemingly similar countries such as Spain and Italy show significant differences in the formal use of care, while the informal use of care is comparable. This may be related to differences in health scores, with ADL and chronic disease scores in particular being significantly worse in Spain, leading to a higher need for formal care. Comparing neighbors Belgium and the Netherlands, the difference in formal care use is even greater. However, health scores here also suggest one of the reasons for these differences. Of course, other important reasons may also influence these differences, such as government spending on long-term care and other sociocultural characteristics. According to the recorded data, diversity is observed in use when choosing care (formal vs. informal). In addition, cultural norms (family-oriented societies) and other parameters (age, income, education, life in rural areas) are also different, which indicates the necessity of creating a system in accordance with dissimilarity at the national level.
4.1 Analysis of inequality
Figure 1 shows the CI values for each country accompanied by bootstrap 95% confidence intervals. The measures whose intervals do not cross zero are significant at 0.05 significance level. CI for most countries is negative, indicating a pro-poor distribution of LTC.
Figure 1Concentration index values for each country DISPLAY Figure
The only statistically significant positive CI is recorded for formal care in Italy, where informal care CI is also significantly negative. The only other positive formal care CIs are for Greece, Malta and Cyprus, all not significantly different from zero.
Informal care CIs are almost uniformly smaller than corresponding formal care CIs, making informal care even more pro-poor than formal care in most countries. Austria, Switzerland, Finland, Latvia, Malta and Slovakia have neither measure significantly different from zero. Greece, Belgium, the Czech Republic, Poland, Slovenia, Lithuania, Cyprus and Romania have only informal care CI significantly pro-poor. All other countries have significantly negative measures, with the smallest formal care CIs being in Netherlands, Sweden, Denmark, France and Hungary, and smallest informal care CIs in Sweden, France, Spain, Croatia, the Czech Republic and Romania. From these results, it appears that in most countries both formal and informal care have an unfavorable distribution, i.e., long-term care tends to be used by the poorer strata of the population. However, informal care is even more disproportionately used by the poor in most cases, which may mean that they do not have adequate access to formal care and need to find other informal means of care.
An important consideration in the CI analysis and also in subsequent analyzes is the issue of sample size. To obtain reliable inferences, each country should have sufficient data for the calculations. Since in this study the sample sizes per country are determined a priori by the SHARE sample and could not be increased by additional data collection, we consider here only the sample sizes post-hoc. The basic formula for sample size is: | n = z2 (p(1 - p)) / d2 | (4) |
4.1.1 Formal and informal care concentration index decomposition
Contributions of factors in concentration index decomposition are presented in figures 2 and 3, and figures 4 and 5 show plots of corresponding elasticity and partial CIs. Negative contribution values indicate the pro-poor contribution of the relevant factor to the overall CI, while positive values present a pro-rich contribution. Figures 4 and 5 have areas shaded with different colors, white marking an area with pro-rich contributions (same sign) and grey areas marking pro-poor contributions (different sign).
Health variables (SP health, ADL, Chronic) uniformly across countries contribute to pro-poor inequality in use of LTC, with larger relative contributions recorded for informal care. Regarding formal care, SP health shows the greatest contributions among the health measures, with countries Sweden, France, Denmark, Germany, Hungary, Slovenia, Estonia and Slovakia having the largest contributions. Informal care shows a similar pattern, with countries Hungary, Spain, Sweden, Luxembourg, Slovakia, Denmark, Netherlands, France and Poland showing greatest pro-poor contribution.
For informal care, ADL is an important contributor among health measures. It can be seen on figures 4 and 5 that health variables, excluding minor negative values for a few countries, have positive elasticities, meaning that larger values for these factors predict greater utilization of LTC, while partial CIs are in general pro-poor, so people with greater health needs are disproportionately more represented among poor population. Therefore, products of elasticity and CI result in pro-poor contributions. Overall, for formal care, health variables dominate the contributions of other non-health variables in: Germany, France, Netherlands, Hungary and Slovenia. With informal care, other non-health factors add greater contributions, with Spain, Netherlands, Sweden, France, Denmark, Hungary, Poland, Luxembourg having the largest relative contributions of health variables.
Besides health variables, other need factors are also Age and Gender. Age greatly contributes to the pro-poor inequality in several countries, both for formal and informal care: Sweden, Denmark, Spain, the Czech Republic, Netherlands, Belgium, Lithuania, Switzerland and Hungary. Estonia and Greece have larger contributions with informal care. Elasticity and partial CI plots show that elasticity is uniformly positive for age, which is expected, as older people will utilize more LTC. Also, partial CIs are negative as older individuals are more represented in the poor population. Sweden has the highest contribution of age, which is due to having the most pro-poor distribution of age and one of the highest elasticities for formal care, and relatively high elasticity for informal care. This could be explained by strong state support of elderly people who, although having markedly lower SES, receive high levels of LTC. Other countries with older age contribution have a similar pattern of elasticity and partial CI.
Variable Gender did not much contribute to the overall CI. Females in most countries are disproportionately represented in the poorer population, while in most countries females utilize more LTC, with only some countries having men use more LTC (Slovenia, Poland, Bulgaria and Slovakia for formal care; Bulgaria, Romania and Croatia for informal care). Relatively largest contributions of gender are recorded in Lithuania, Finland and Slovenia for formal care, and the Czech Republic, Hungary and Switzerland for informal care.
Figure 2Formal care concentration index decomposition DISPLAY Figure Figure 3Informal care concentration index decomposition DISPLAY Figure Figure 4Formal care concentration index decomposition DISPLAY Figure Figure 5Informal care concentration index decomposition DISPLAY Figure
As for non-need factors, for most countries the greatest contributions were recorded for Income, followed by Education, Married and Area. Income has by definition a positive partial CI (higher income is more concentrated among richer individuals), so the sign of contribution depends on the sign of elasticity.
Regarding formal care, most countries have positive elasticity, giving pro-poor contributions. Largest positive contributions were recorded for Cyprus (although small sample size makes these values less reliable), Belgium, Italy, Slovenia and Poland. This is of course due to positive associations between income levels and formal care use (positive elasticity). Countries that displayed negative contributions of income were Luxembourg, Croatia, Bulgaria, Finland and Hungary. For these countries, higher income is associated with lower levels of formal care use, which could be because lower income individuals are favored in state support, while higher income individuals find other means of meeting their needs. With informal care income contributions, for the most countries the trend is more negative, with many more countries showing a pronounced pro-poor contribution, like Romania, Cyprus, Croatia, Germany, Italy, Bulgaria, Sweden, Luxembourg, Slovenia and Latvia. For these countries informal care is more utilized among the poor, driving pro-poor inequality. Of the countries with pro-rich contributions, most pronounced are Slovakia (also small sample size so less reliable), Finland, Hungary, Netherlands, Switzerland and Greece, as here there is higher utilization of informal care by richer individuals.
Education is similar to income in terms of elasticity and partial CI, with all countries having a pro-rich partial CI, and elasticity defining the sign of contribution. Education shows a smaller contribution than Income for most countries, with largest pro-rich contributions in formal care recorded for Italy, Luxembourg, Lithuania, Cyprus and Belgium, while Slovakia, Poland, Finland and Slovenia showed a pro-poor contribution. Interestingly, Slovakia and Poland have opposite signs of income and education contributions, which could be because here the Area factor is more pronounced, explaining some variation for the rural, less educated population, while the other part is explained by income which correlates with education, so education elasticity has a negative sign. Regarding informal care, education elasticity for most countries is negative, giving pronounced pro-rich contributions only for Germany and Sweden, while most other countries have pro-poor contributions, although relatively unimportant compared to other factors, except for Malta, Slovenia and Italy.
Area was not an important contributor for formal care in most countries, except to some extent in Slovakia, Romania, Poland, Hungary and Greece. Most contributions were pro-rich, as most countries have poorer rural areas and less utilization of LTC in such areas, with Hungary being one of the exceptions with greater utilization recorded for rural areas. Informal care showed somewhat similar pattern, with both positive and negative contributions. Relatively largest contributions were recorded for Cyprus, Slovakia and Hungary.
Last group of factors are Married and Children. For most countries, including both formal and informal care, these two factors were not important contributors to inequality, with Children being mostly negligible, except for Malta (formal care). All contributions of being married were pro-poor, owing to partial CI being pro-rich (married people are disproportionately represented among richer population) and elasticity predominantly negative, both for formal and informal care, meaning that married people use less LTC. Largest contributions in formal care were recorded for Romania (where other contributions dominate), the Czech Republic, Sweden, Estonia and Latvia, while informal care contributions were the largest for Sweden, Denmark, Belgium, Czech Republic, France, Finland and Romania. Informal care contributions were more pronounced than formal, and in more countries, implying that being married results in less use of informal care.
4.2 Inequity analysis
Previous results of decomposition showed that need factors greatly contributed to the pro-poor inequality for most countries. These factors can be defined as legitimate sources of inequality in LTC utilization, so with an analysis of equity we measure inequality after accounting for need factors. Figure 6 shows horizontal inequity indices for all countries with corresponding bootstrapped 95% confidence intervals.
Figure 6 shows that for most countries HI is more positive than CI, and many previously significant pro-poor concentration indices are now not significantly different from zero. A significantly pro-rich HI was recorded for Italy, Greece, Belgium and Cyprus for formal care, and Slovakia for informal care, and a significantly pro-poor HI for Luxembourg and Croatia for formal care, and Germany, Sweden, Italy, France, Denmark, Belgium, Luxembourg, Slovenia, Croatia, Bulgaria, Cyprus and Romania for informal care.
After accounting for need factors, formal care inequalities disappeared for most countries, while informal care inequalities remained in much greater number for most countries, mostly with pro-poor orientation. The inequality analysis shows that formal care use is more evenly distributed after accounting for legitimate sources of inequality than the CI analysis showed, so that inequality between the poor and CIs in many countries is mainly driven by legitimate sources of need. On the other hand, the use of informal care, although less pronounced than the CI distribution, is still pro-poor oriented, which in turn means that poorer people who cannot use formal care resort to informal sources even after accounting for need factors. A notable exception is Slovakia, where HI is even more pro-rich than the corresponding CI.
Figure 6Horizontal inequity DISPLAY Figure
5 Conclusion and discussion
These findings lend considerable importance to the existing scientific approach to the long-term sector in relation to home care. The differences in the use of home care show that there is diversity among the 27 EU member states and that the use of home care is determined by a sum of need and non-need factors in the region that may influence the choice of care used. In addition, differences among income groups within EU-27 members and within countries themselves were found, even when controlling for need factors. Thus, it was possible to determine which factors cause inequality between socioeconomic groups in home care.
This study provides an overview of horizontal income inequality in the availability of home care among 27 European Union countries. In addition to using the most recent SHARE data collected last year, this study included, to our knowledge, the largest number of countries analyzed using traditionally developed methods for inequality. The problem of inequality has been previously addressed by authors Ilinca et al., (  2017 2017); Rodrigues, Ilinca and Schmidt (  2017 2017) using data from previous editions of SHARE and with a smaller number of countries observed in Europe. Our study confirms the findings of the aforementioned authors that a pro-poor distribution of long-term care prevails in most countries of the EU-27. In addition, due to the large volume of countries included in the research and the lack of relevant literature dealing with horizontal inequality in long-term care for the elderly, we believe that this study will make a great contribution to the consideration of sufficient equal services for the same group of users. Also, the latest data provide a clear overview of the current state of the use of formal and informal care in the European Union, which is of crucial importance in planning policies for the care of elderly people. Although we are aware that due to the market economy, it is not in the interest of countries to have perfect equality, we wanted to investigate which countries are close to this concept, that is, how formal and informal care are distributed within the EU member states in accordance with the level of income of individuals. It is particularly important to emphasize that at the very beginning of this analysis, the member states are not in the same starting position. Take, for example, the countries of the Balkans, where, due to the former communist regimes and stronger family attachment, there is a stronger preference for an informal form of care. The formal form is an alternative form of long-term care for the majority of users due to smaller national generosity (smaller grants) and greater reliance on family financial support.
Based on analysis of inequality, pro-poor distribution of LTC was indicated in most of the observed countries, which is consistent with the previous research (Ilinca et al.,  2017 2017). Health variables across countries contribute to pro-poor inequality in use of LTC, mainly for informal care. People with greater health needs are disproportionately more represented among poor population. Age greatly contributes to the pro-poor inequality in several countries, both for formal and informal care. The Gender variable did not much contribute to the overall CI. Females in most countries are disproportionately represented in the poorer population, while in most countries females utilize more LTC, which is consistent with other research on the subject (Forma et al.,  2007 2007;  2017 2017). Regarding formal care, most countries have pro-poor contributions but surprisingly for some countries higher income is associated with lower levels of formal care use, which could be the result of lower income individuals being favored in state support, while higher income individuals find other means of meeting their needs. The Education variable shows all countries having a pro-rich partial CI, which can be seen as more educated people experience fewer inequalities. Education and Income are in positive correlation, which means that higher-educated people enjoy better income. Bearing in mind that a pro-poor distribution is presented in the use of formal and informal care in European Union among elderly people, our initial hypothesis is accepted. Most contributions of the Area variable were pro-rich, as most countries have poorer rural areas and less utilization of LTC in such areas, probably because most countries have centralized systems of care placed in better developed areas. After accounting for need factors, formal care inequalities disappeared for most countries, while informal care inequalities remained in much greater numbers for most countries, mostly with pro-poor orientation.
6 Limitations
Two criteria were excluded from the analyzed sample: persons younger than 65 years of age and persons who have a permanent residence in long-term care institutions. Institutional care is understood as care for an elderly person in homes for the elderly or in any other facility of a formal nature (assisted living, day care) without including a stay in one’s own home. It is characteristic for people who are institutionalized to have a high rate of morbidity and seriously impaired health, which can influence the underestimation of the connection of certain variables to the final outcome. When considering the sample, the mortality rate was not included (people of lower standards who live in rural areas have a shorter life expectancy), which can affect the outcome of the results.
The next type of limitation is the small representative sample, which may affect the study outcome results. Regarding sample sizes in relation to HI, most of the same conclusions given for CI hold here. Bootstrapped confidence intervals for HI are comparable to those for CI, so the problems with sample size pointed out in the CI section should here also be taken into consideration.
In addition, when talking about the health status of users, it should be kept in mind that this is a subjective perception by the participants of the long-term SHARE study. The study used total household income as a measure of total income, as opposed to equivalent income or per capita income, which are used in various scientific studies. Although some authors state net worth as more adequate, income, due to its measurability, variability (transition from working income to pensions) and frequency (the most common measurable data when expressing socioeconomic inequalities) represents a better choice for measuring the availability of long-term care among elderly people.
Funding
The publication of this paper has been supported by University of Rijeka under the project Smart cities in function of the development of the national economy (uniri-drustv-18-255-1424).
Notes
* The authors are grateful to two anonymous referees who have contributed to the quality of the final version of the paper.
1 Niko Speybroeck Decomposing socioeconomic health inequalities, Int J Public Health (2010) 55:347-351.
* The authors are grateful to two anonymous referees who have contributed to the quality of the final version of the paper.
1 Niko Speybroeck Decomposing socioeconomic health inequalities, Int J Public Health (2010) 55:347-351.
Disclosure statement
The authors disclose any financial or other substantive conflict of interest that might be construed as influencing the results or interpretation of the paper or state that they do not have any conflict of interest.
Acknowledgements This paper uses data from SHARE Waves 1, 2, 3, 4, 5, 6, 7, 8 and 9 (DOIs: 10.6103/SHARE.w1.800, 10.6103/SHARE.w2.800, 10.6103/SHARE.w3.800, 10.6103/SHARE.w4.800, 10.6103/SHARE.w5.800, 10.6103/SHARE.w6.800, 10.6103/SHARE.w7.800, 10.6103/SHARE.w8.800, 10.6103/SHARE.w8ca.800, 10.6103/SHARE.w9ca800, see Börsch-Supan et al. (  2013 2013) for methodological details.(1)The SHARE data collection has been funded by the European Commission, DG RTD through FP5 (QLK6-CT-2001-00360), FP6 (SHARE-I3: RII-CT-2006-062193, COMPARE: CIT5-CT-2005-028857, SHARELIFE: CIT4- CT-2006-028812), FP7 (SHARE-PREP: GA N°211909, SHARE-LEAP: GA N°227822, SHARE M4: GA N°261982, DASISH: GA N°283646) and Horizon 2020 (SHARE-DEV3: GA N°676536, SHARE-COHESION: GA N°870628, SERISS: GA N°654221, SSHOC: GA N°823782, SHARE-COVID19: GA N°101015924) and by DG Employment, Social Affairs & Inclusion through VS 2015/0195, VS 2016/0135, VS 2018/0285, VS 2019/0332, and VS 2020/0313. Additional funding from the German Ministry of Education and Research, the Max Planck Society for the Advancement of Science, the U.S. National Institute on Aging (U01_ AG09740-13S2, P01_AG005842, P01_AG08291, P30_AG12815, R21_AG025169, Y1-AG-4553-01, IAG_BSR06-11, OGHA_04-064, HHSN271201300071C, RAG052527A) and from various national funding sources is gratefully acknowledged.
References
Albertini, M. and Pavolini, E., 2017. Unequal inequalities: The stratification of the use of formal care among older Europeans. J ournals of Gerontology - Series B Psychological Sciences and Social Sciences, 72(3), pp. 510-521 [ CrossRef]
Bago d’Uva, T., Jones, A. M. and van Doorslaer, E., 2009. Measurement of horizontal inequity in health care utilization using European panel data. Journal of Health Economics, 28(2), pp. 280-289 [ CrossRef]
Barbieri, D. and Ghibelli, P. (eds.), 2018. Formal Versus Informal Long-term Care: Economic and Social Impacts [ CrossRef]
Bonsang, E., 2009. Does informal care from children to their elderly parents substitute for formal care in Europe? Journal of Health Economics, 28(1), pp. 143-154 [ CrossRef]
Börsch-Supan, A. [et al.], 2013. Data Resource Profile: The Survey of Health, Ageing and Retirement in Europe (SHARE) [ CrossRef]
Börsch-Supan, A., 2022. Survey of Health, Ageing and Retirement in Europe (SHARE) Wave 8. Release version: 8.0.0. SHARE-ERIC [ CrossRef]
Brackley, M. E. and Penning, M. J., 2009. Home-care utilization within the year of death: Trends, predictors and changes in access equity during a period of health policy reform in British Columbia, Canada. Health and Social Care in the Community, 17(3), pp. 283-294 [ CrossRef]
Broese van Groenou, M. I. [et al.], 2006. Socio-economic status differences in older people’s use of informal and formal help: A comparison of four European countries. Ageing and Society, 26(5), pp. 745-766 [ CrossRef]
Broese van Groenou, M. I. and de Boer, A., 2016. Providing informal care in a changing society. European Journal of Ageing, 13, pp. 271-279 [ CrossRef]
Carrieri, V. and Bilger, M., 2013. Preventive care: Underused even when free. Is there something else at work? Applied Economics, 45(2), pp. 239-253 [ CrossRef]
Carrieri, V. and Wuebker, A., 2013. Assessing inequalities in preventive care use in Europe. Health Policy, 113(3), pp. 247-257 [ CrossRef]
Carrieri, V., di Novi, C. and Orso, C. E., 2017. Home Sweet Home? Public Financing and Inequalities in the Use of Home Care Services in Europe. Fiscal Studies, 38(3), 445-468 [ CrossRef]
Chuakhamfoo, N. N. [et al.], 2020. Health and long-term care of the elderly with dementia in rural Thailand: A cross-sectional survey through their caregivers. BMJ Open, 10(3), pp. 1-11 [ CrossRef]
Erreygers, G., 2009. Correcting the Concentration Index. Journal of Health Economics, 28(2), pp. 504-515 [ CrossRef]
Fernandez, J. L. and Forder, J., 2015. Local variability in long-term care services: Local autonomy, exogenous influences and policy spillovers. Health Economics (United Kingdom), 24(S1), pp. 146-157 [ CrossRef]
Forma, L. [et al.], 2007. Health and social service use among old people in the last 2 years of life. European Journal of Ageing, 4(3), pp. 145-154 [ CrossRef]
Forma, L. [et al.], 2017. Trends in the use and costs of round-the-clock long-term care in the last two years of life among old people between 2002 and 2013 in Finland. BMC Health Services Research, 17(1) [ CrossRef]
Ilinca, S. [et al.], 2017. Fairness and Eligibility to Long-Term Care: An Analysis of the Factors Driving Inequality and Inequity in the Use of Home Care for Older Europeans. International Journal of Environmental Research and Public Health, 14(10) [ CrossRef]
Lera, J., Pascual-Sáez, M. and Cantarero-Prieto, D., 2021. Socioeconomic Inequality in the Use of Long-Term Care among European Older Adults: An Empirical Approach Using the SHARE Survey. International Journal of Environmental Research and Public Health, 18(1) [ CrossRef]
Penning, M. J. [et al.], 2018. Long-term care trajectories in Canadian context: Patterns and predictors of publicly funded care. Journals of Gerontology - Series B Psychological Sciences and Social Sciences, 73(6), pp. 1077-1087 [ CrossRef]
Rehnberg, J. and Fritzell, J., 2016. The shape of the association between income and mortality in old age: A longitudinal Swedish national register study. SSM - Population Health, 2, pp. 750-756 [ CrossRef]
Rodrigues, R., Ilinca, S. and Schmidt, A. E., 2017. Inequality and inequity in the use of long-term care services in Europe: is there reason for concern? Eurohealth, 23(4), pp. 7-10.
Saito, T. [et al.], 2018. Income-based inequalities in caregiving time and depressive symptoms among older family caregivers under the Japanese long-term care insurance system: A cross-sectional analysis. PLoS ONE, 13(3) [ CrossRef]
Sarasa, S. and Bilingsley, S., 2008. Personal and household care giving from adult children to parents and social stratification. In C. Saraceno, ed. Families, Ageing and Social Policy. Cheltenham: Edward Elgar, pp. 123-146.
Tenand, M., Bakx, P. and van Doorslaer, E., 2020. Equal long-term care for equal needs with universal and comprehensive coverage? An assessment using Dutch administrative data. Health Economics, 29(4), pp. 435-451 [ CrossRef]
van de Poel, E., van Doorslaer, E. and O’Donnell, O., 2012. Measurement of inequity in health care with heterogeneous response of use to need. Journal of Health Economics, 31(4), pp. 676-689 [ CrossRef]
van Deurzen, I., van Oorschot, W. and van Ingen, E., 2014. The Link between Inequality and Population Health in Low and Middle Income Countries: Policy Myth or Social Reality? [ CrossRef]
van Doorslaer, E., Koolman, X. and Jones, A. M., 2004. Explaining income-related inequalities in doctor utilization in Europe. Health Economics, 13(7), pp. 629-647 [ CrossRef]
Wagstaff, A. and van Doorslaer, E., 2000. The Board of Regents of the University of Wisconsin System Measuring and Testing for Inequity in the Delivery of Health Care Measuring and Testing for Inequity in the Delivery of Health Care. The Journal of Human Resources, 35(4), pp. 716-733 [ CrossRef]
Wagstaff, A., van Doorslaer, E. and Paci, P., 1991. On the measurement of horizontal inequity in the delivery of health care. Journal of Health Economics, 10(2), pp. 169-205 [ CrossRef]
Albertini, M. and Pavolini, E., 2017. Unequal inequalities: The stratification of the use of formal care among older Europeans. J ournals of Gerontology - Series B Psychological Sciences and Social Sciences, 72(3), pp. 510-521 [ CrossRef]
Bago d’Uva, T., Jones, A. M. and van Doorslaer, E., 2009. Measurement of horizontal inequity in health care utilization using European panel data. Journal of Health Economics, 28(2), pp. 280-289 [ CrossRef]
Barbieri, D. and Ghibelli, P. (eds.), 2018. Formal Versus Informal Long-term Care: Economic and Social Impacts [ CrossRef]
Bonsang, E., 2009. Does informal care from children to their elderly parents substitute for formal care in Europe? Journal of Health Economics, 28(1), pp. 143-154 [ CrossRef]
Börsch-Supan, A. [et al.], 2013. Data Resource Profile: The Survey of Health, Ageing and Retirement in Europe (SHARE) [ CrossRef]
Börsch-Supan, A., 2022. Survey of Health, Ageing and Retirement in Europe (SHARE) Wave 8. Release version: 8.0.0. SHARE-ERIC [ CrossRef]
Brackley, M. E. and Penning, M. J., 2009. Home-care utilization within the year of death: Trends, predictors and changes in access equity during a period of health policy reform in British Columbia, Canada. Health and Social Care in the Community, 17(3), pp. 283-294 [ CrossRef]
Broese van Groenou, M. I. [et al.], 2006. Socio-economic status differences in older people’s use of informal and formal help: A comparison of four European countries. Ageing and Society, 26(5), pp. 745-766 [ CrossRef]
Broese van Groenou, M. I. and de Boer, A., 2016. Providing informal care in a changing society. European Journal of Ageing, 13, pp. 271-279 [ CrossRef]
Carrieri, V. and Bilger, M., 2013. Preventive care: Underused even when free. Is there something else at work? Applied Economics, 45(2), pp. 239-253 [ CrossRef]
Carrieri, V. and Wuebker, A., 2013. Assessing inequalities in preventive care use in Europe. Health Policy, 113(3), pp. 247-257 [ CrossRef]
Carrieri, V., di Novi, C. and Orso, C. E., 2017. Home Sweet Home? Public Financing and Inequalities in the Use of Home Care Services in Europe. Fiscal Studies, 38(3), 445-468 [ CrossRef]
Chuakhamfoo, N. N. [et al.], 2020. Health and long-term care of the elderly with dementia in rural Thailand: A cross-sectional survey through their caregivers. BMJ Open, 10(3), pp. 1-11 [ CrossRef]
Erreygers, G., 2009. Correcting the Concentration Index. Journal of Health Economics, 28(2), pp. 504-515 [ CrossRef]
Fernandez, J. L. and Forder, J., 2015. Local variability in long-term care services: Local autonomy, exogenous influences and policy spillovers. Health Economics (United Kingdom), 24(S1), pp. 146-157 [ CrossRef]
Forma, L. [et al.], 2007. Health and social service use among old people in the last 2 years of life. European Journal of Ageing, 4(3), pp. 145-154 [ CrossRef]
Forma, L. [et al.], 2017. Trends in the use and costs of round-the-clock long-term care in the last two years of life among old people between 2002 and 2013 in Finland. BMC Health Services Research, 17(1) [ CrossRef]
Ilinca, S. [et al.], 2017. Fairness and Eligibility to Long-Term Care: An Analysis of the Factors Driving Inequality and Inequity in the Use of Home Care for Older Europeans. International Journal of Environmental Research and Public Health, 14(10) [ CrossRef]
Lera, J., Pascual-Sáez, M. and Cantarero-Prieto, D., 2021. Socioeconomic Inequality in the Use of Long-Term Care among European Older Adults: An Empirical Approach Using the SHARE Survey. International Journal of Environmental Research and Public Health, 18(1) [ CrossRef]
Penning, M. J. [et al.], 2018. Long-term care trajectories in Canadian context: Patterns and predictors of publicly funded care. Journals of Gerontology - Series B Psychological Sciences and Social Sciences, 73(6), pp. 1077-1087 [ CrossRef]
Rehnberg, J. and Fritzell, J., 2016. The shape of the association between income and mortality in old age: A longitudinal Swedish national register study. SSM - Population Health, 2, pp. 750-756 [ CrossRef]
Rodrigues, R., Ilinca, S. and Schmidt, A. E., 2017. Inequality and inequity in the use of long-term care services in Europe: is there reason for concern? Eurohealth, 23(4), pp. 7-10.
Saito, T. [et al.], 2018. Income-based inequalities in caregiving time and depressive symptoms among older family caregivers under the Japanese long-term care insurance system: A cross-sectional analysis. PLoS ONE, 13(3) [ CrossRef]
Sarasa, S. and Bilingsley, S., 2008. Personal and household care giving from adult children to parents and social stratification. In C. Saraceno, ed. Families, Ageing and Social Policy. Cheltenham: Edward Elgar, pp. 123-146.
Tenand, M., Bakx, P. and van Doorslaer, E., 2020. Equal long-term care for equal needs with universal and comprehensive coverage? An assessment using Dutch administrative data. Health Economics, 29(4), pp. 435-451 [ CrossRef]
van de Poel, E., van Doorslaer, E. and O’Donnell, O., 2012. Measurement of inequity in health care with heterogeneous response of use to need. Journal of Health Economics, 31(4), pp. 676-689 [ CrossRef]
van Deurzen, I., van Oorschot, W. and van Ingen, E., 2014. The Link between Inequality and Population Health in Low and Middle Income Countries: Policy Myth or Social Reality? [ CrossRef]
van Doorslaer, E., Koolman, X. and Jones, A. M., 2004. Explaining income-related inequalities in doctor utilization in Europe. Health Economics, 13(7), pp. 629-647 [ CrossRef]
Wagstaff, A. and van Doorslaer, E., 2000. The Board of Regents of the University of Wisconsin System Measuring and Testing for Inequity in the Delivery of Health Care Measuring and Testing for Inequity in the Delivery of Health Care. The Journal of Human Resources, 35(4), pp. 716-733 [ CrossRef]
Wagstaff, A., van Doorslaer, E. and Paci, P., 1991. On the measurement of horizontal inequity in the delivery of health care. Journal of Health Economics, 10(2), pp. 169-205 [ CrossRef]
|








 2021
2021