4376
Views
971
Downloads |
Why are older informal carers in better health? Solving a causality problem
Preliminary communication | Year: 2018 | Pages: 303 - 323 | Volume: 42 | Issue: 3 Received: May 23, 2018 | Accepted: July 12, 2018 | Published online: September 3, 2018
|

FULL ARTICLE
FIGURES & DATA
REFERENCES
CROSSMARK POLICY
METRICS
LICENCING
PDF
|
|
Country
|
Helpgiving_tot
|
Helpgiving_out
|
Helpgiving_wtin
|
|
Scand
|
Sweden
|
1,527,567
|
1,460,927
|
113,159
|
|
Denmark
|
1,048,569
|
1,005,553
|
92,927
|
|
Netherlands
|
2,376,857
|
2,163,370
|
315,709
|
|
Contin
|
Austria
|
953,164
|
833,773
|
177,566
|
|
Belgium
|
1,637,570
|
1,426,540
|
331,931
|
|
France
|
8,371,773
|
7,252,966
|
1,507,020
|
|
Germany
|
12,648,003
|
11,455,470
|
1,745,328
|
|
Luxembourg
|
52,710
|
45,376
|
10,395
|
|
Switzerland
|
839,445
|
790,900
|
90,097
|
|
Medit
|
Italy
|
7,153,458
|
6,053,197
|
1,691,223
|
|
Spain
|
3,572,164
|
2,512,323
|
1,268,977
|
|
East
|
Czech Republic
|
1,483,696
|
1,341,115
|
298,467
|
|
Estonia
|
172,302
|
150,356
|
36,329
|
|
Slovenia
|
131,627
|
106,774
|
39,095
|
|
Mix
|
Israel
|
306,143
|
198,250
|
119,050
|
|
Tot
|
Total
|
42,275,048
|
36,796,889
|
7,837,273
|
|
Probit: Help_outside
|
Coeff.
|
z
|
P>z
|
Coeff.
|
z
|
P>z
|
Coeff.
|
z
|
P>z
|
|
Gender
|
0.0095
|
0.84
|
|
0.0104
|
0.91
|
|
-0.0016
|
-0.14
|
|
|
Age
|
-0.0239
|
-28.51
|
***
|
-0.0234
|
-28.12
|
***
|
-0.0233
|
-27.80
|
***
|
|
Edu_Years
|
0.0190
|
13.59
|
***
|
0.0190
|
13.61
|
***
|
0.0191
|
13.63
|
***
|
|
Income_Middle
|
0.0371
|
2.67
|
***
|
0.0373
|
2.69
|
***
|
0.0392
|
2.81
|
***
|
|
Income_Upper
|
0.1028
|
7.19
|
***
|
0.1026
|
7.16
|
***
|
0.1077
|
7.48
|
***
|
|
Retired vs. Employed
|
0.0789
|
4.76
|
***
|
0.0818
|
4.94
|
***
|
0.0789
|
4.75
|
***
|
|
Other vs. Employed
|
-0.0225
|
-1.20
|
|
-0.0162
|
-0.87
|
|
-0.0260
|
-1.38
|
|
|
Hh_Size
|
-0.0514
|
-8.12
|
***
|
-0.0513
|
-8.11
|
***
|
-0.0510
|
-8.02
|
***
|
|
Physical_Inactivity
|
-0.3691
|
-16.73
|
***
|
-0.3638
|
-16.52
|
***
|
-0.3883
|
-17.27
|
***
|
|
Memory
|
0.0377
|
13.23
|
***
|
0.0369
|
12.91
|
***
|
0.0384
|
13.33
|
***
|
|
Continental
|
0.1064
|
7.68
|
***
|
0.1045
|
7.51
|
***
|
0.1037
|
7.43
|
***
|
|
Socialdemocratic
|
0.4534
|
25.15
|
***
|
0.4553
|
24.65
|
***
|
0.4624
|
25.46
|
***
|
|
Mediterranean
|
-0.1866
|
-9.79
|
***
|
-0.1893
|
-9.93
|
***
|
-0.1897
|
-9.90
|
***
|
|
Chronic diseases
|
0.0404
|
3.50
|
***
|
|
|
|
|
|
|
|
Self-rated Health
|
|
|
|
0.0077
|
0.60
|
|
|
|
|
|
Depression
|
|
|
|
|
|
|
0.1052
|
7.93
|
***
|
|
Constant
|
0.5855
|
8.89
|
***
|
0.5676
|
8.53
|
***
|
0.5541
|
8.35
|
***
|
|
Observations
|
62257
|
|
|
62330
|
|
|
61547
|
|
|
|
LR Chi2
|
5073.81
|
***
|
|
5032.93
|
***
|
|
5001.36
|
***
|
|
|
Pseudo R2
|
0.0673
|
|
|
0.0667
|
|
|
0.0670
|
|
|
|
Log Likelihood
|
-35168.70
|
|
|
-35221.55
|
|
|
-34847.12
|
|
|
|
Help_total
|
Coeff.
|
z
|
P>z
|
Coeff.
|
z
|
P>z
|
Coeff.
|
z
|
P>z
|
|
Gender
|
0.0246
|
2.72
|
***
|
0.0183
|
2.11
|
**
|
0.0282
|
2.82
|
***
|
|
Age
|
-0.0071
|
-10.03
|
***
|
-0.0078
|
-12.34
|
***
|
-0.0079
|
-12.62
|
***
|
|
Edu_Years
|
0.0030
|
2.86
|
***
|
0.0028
|
2.64
|
***
|
0.0032
|
3.07
|
***
|
|
Income_Middle
|
0.0133
|
1.33
|
|
0.0108
|
1.09
|
|
0.0132
|
1.33
|
|
|
Income_Upper
|
0.0161
|
1.45
|
|
0.0124
|
1.10
|
|
0.0174
|
1.57
|
|
|
Retired vs. Employed
|
0.0258
|
1.69
|
*
|
0.0159
|
1.16
|
|
0.0068
|
0.52
|
|
|
Other vs. Employed
|
0.0112
|
0.60
|
|
-0.0013
|
-0.08
|
|
-0.0088
|
-0.56
|
|
|
Hh_Size
|
0.0026
|
0.48
|
|
0.0022
|
0.40
|
|
0.0021
|
0.37
|
|
|
Physical_Inactivity
|
-0.0391
|
-2.30
|
**
|
-0.0504
|
-3.29
|
***
|
-0.0439
|
-2.62
|
***
|
|
Memory
|
0.0061
|
2.69
|
***
|
0.0060
|
2.60
|
***
|
0.0065
|
2.86
|
***
|
|
Continental
|
-0.0140
|
-0.77
|
|
-0.0042
|
-0.25
|
|
0.0037
|
0.22
|
|
|
Socialdemocratic
|
0.0652
|
3.42
|
***
|
0.0512
|
2.40
|
**
|
0.0784
|
4.36
|
***
|
|
Mediterranean
|
-0.0669
|
-3.41
|
***
|
-0.0553
|
-3.00
|
***
|
-0.0471
|
-2.53
|
**
|
|
Chronic diseases
|
-0.1309
|
-2.49
|
**
|
|
|
|
|
|
|
|
Self-rated Health
|
|
|
|
-0.0936
|
-2.46
|
**
|
|
|
|
|
Depression
|
|
|
|
|
|
|
-0.0739
|
-1.97
|
**
|
|
Constant
|
0.7908
|
14.58
|
***
|
0.8617
|
14.07
|
***
|
0.7942
|
14.63
|
***
|
|
Observations
|
13232
|
|
|
13179
|
|
|
13149
|
|
|
|
Wald Chi2
|
650.65
|
***
|
|
660.09
|
***
|
|
654.60
|
***
|
|
|
Log Likelihood
|
-17116.06
|
|
|
-15074.79
|
|
|
-14999.20
|
|
|
|
Test of endogeneity
|
7.04
|
***
|
|
4.87
|
**
|
|
8.52
|
***
|
|
|
Help_outside
|
Coeff.
|
z
|
P>z
|
Coeff.
|
z
|
P>z
|
Coeff.
|
z
|
P>z
|
|
Gender
|
0.0136
|
1.57
|
|
0.0055
|
0.66
|
|
0.0235
|
2.5
|
**
|
|
Age
|
-0.0083
|
-12.56
|
***
|
-0.0093
|
-15.51
|
***
|
-0.0095
|
-15.75
|
***
|
|
Edu_Years
|
0.0039
|
3.92
|
***
|
0.0038
|
3.81
|
***
|
0.0041
|
4.14
|
***
|
|
Income_Middle
|
0.0096
|
1.00
|
|
0.0070
|
0.74
|
|
0.0077
|
0.8
|
|
|
Income_Upper
|
0.0163
|
1.53
|
|
0.0144
|
1.35
|
|
0.0165
|
1.55
|
|
|
Retired vs. Employed
|
0.0333
|
2.34
|
**
|
0.0156
|
1.21
|
|
0.0086
|
0.68
|
|
|
Other vs. Employed
|
0.0131
|
0.76
|
|
-0.0092
|
-0.59
|
|
-0.0103
|
-0.68
|
|
|
Hh_Size
|
-0.0275
|
-5.19
|
***
|
-0.0277
|
-5.23
|
***
|
-0.0288
|
-5.39
|
***
|
|
Physical_Inactivity
|
-0.0488
|
-3.07
|
***
|
-0.0690
|
-4.78
|
***
|
-0.0465
|
-2.94
|
***
|
|
Memory
|
0.0086
|
3.97
|
***
|
0.0092
|
4.28
|
***
|
0.0082
|
3.77
|
***
|
|
Continental
|
-0.0139
|
-0.81
|
|
0.0033
|
0.21
|
|
0.0131
|
0.83
|
|
|
Socialdemocratic
|
0.0780
|
4.31
|
***
|
0.0727
|
3.74
|
***
|
0.0965
|
5.6
|
***
|
|
Mediterranean
|
-0.0799
|
-4.30
|
***
|
-0.0624
|
-3.56
|
***
|
-0.0491
|
-2.75
|
***
|
|
Chronic diseases
|
-0.1749
|
-3.92
|
***
|
|
|
|
|
|
|
|
Self-rated Health
|
|
|
|
-0.0839
|
-2.74
|
**
|
|
|
|
|
Depression
|
|
|
|
|
|
|
-0.1404
|
-4.24
|
***
|
|
Constant
|
0.9109
|
17.49
|
***
|
0.9716
|
17.21
|
***
|
0.9227
|
17.71
|
***
|
|
Observations
|
13236
|
|
|
13183
|
|
|
13153
|
|
|
|
Wald Chi2
|
1036.86
|
***
|
|
1062.89
|
***
|
|
1053.86
|
***
|
|
|
Log Likelihood
|
-16505.67
|
|
|
-14463.15
|
|
|
-14398.63
|
|
|
|
Test of endogeneity
|
14.92
|
***
|
|
5.08
|
**
|
|
18.90
|
***
|
|
|
Help_within
|
Coeff.
|
z
|
P>z
|
Coeff.
|
z
|
P>z
|
Coeff.
|
z
|
P>z
|
|
Gender
|
0.0297
|
2.63
|
***
|
0.0136
|
1.34
|
|
0.0281
|
2.76
|
***
|
|
Age
|
0.0018
|
2.36
|
**
|
0.0013
|
1.86
|
*
|
0.0019
|
2.91
|
***
|
|
Edu_Years
|
-0.0010
|
-0.74
|
|
-0.0014
|
-1.12
|
|
-0.0004
|
-0.33
|
|
|
Income_Middle
|
0.0042
|
0.34
|
|
-0.0083
|
-0.73
|
|
0.0002
|
0.02
|
|
|
Income_Upper
|
-0.0237
|
-1.65
|
*
|
-0.0407
|
-3.15
|
***
|
-0.0131
|
-1.09
|
|
|
Retired vs. Employed
|
0.0682
|
3.56
|
***
|
0.0382
|
2.23
|
**
|
-0.0008
|
-0.05
|
|
|
Other vs. Employed
|
0.0833
|
3.96
|
***
|
0.0509
|
2.70
|
***
|
0.0030
|
0.18
|
|
|
Hh_Size
|
0.0182
|
3.01
|
***
|
0.0188
|
3.25
|
***
|
0.0273
|
4.19
|
***
|
|
Physical_Inactivity
|
0.0518
|
3.32
|
***
|
0.0389
|
2.77
|
***
|
0.0086
|
0.62
|
|
|
Memory
|
-0.0055
|
-1.97
|
**
|
-0.0055
|
-2.21
|
**
|
-0.0011
|
-0.46
|
|
|
Receiving_help
|
0.1061
|
7.36
|
***
|
0.0819
|
5.88
|
***
|
0.0902
|
5.87
|
***
|
|
Continental
|
-0.1043
|
-5.39
|
***
|
-0.0729
|
-4.20
|
***
|
-0.0532
|
-3.32
|
***
|
|
Socialdemocratic
|
-0.1090
|
-4.92
|
***
|
-0.1615
|
-8.06
|
***
|
-0.0792
|
-4.32
|
***
|
|
Mediterranean
|
-0.0548
|
-2.54
|
**
|
-0.0404
|
-2.09
|
**
|
-0.0260
|
-1.41
|
|
|
Chronic diseases
|
-0.4332
|
-34.91
|
***
|
|
|
|
|
|
|
|
Self-rated Health
|
|
|
|
-0.4326
|
-36.13
|
***
|
|
|
|
|
Depression
|
|
|
|
|
|
|
0.0119
|
0.36
|
|
|
Constant
|
0.2021
|
3.08
|
***
|
0.3982
|
6.60
|
***
|
-0.0962
|
-1.68
|
*
|
|
Observations
|
4656
|
|
|
4634
|
|
|
4615
|
|
|
|
Wald Chi2
|
1318.33
|
***
|
|
1397.63
|
***
|
|
136.85
|
***
|
|
|
Log Likelihood
|
-3592.05
|
|
|
-2002.05
|
|
|
-3583.52
|
|
|
|
Test of endogeneity
|
299.29
|
***
|
|
525.46
|
***
|
|
0.38
|
|
|
Source: Own calculations.
|
|
Help_total
|
Help_outside
|
Help_within
|
|
Chronic diseases
|
-0.1545
|
***
|
-0.1837
|
***
|
-0.5459
|
***
|
|
Self-rated Health
|
-0.1095
|
***
|
-0.1108
|
***
|
-0.5537
|
***
|
|
Depression
|
-0.0939
|
**
|
-0.1559
|
***
|
0.0130
|
|
|
|
|
|
|
|
|
|
|
Help_total
|
Help_outside
|
Help_within
|
|
Chronic diseases
|
-0.1493
|
***
|
-0.1924
|
***
|
-0.6022
|
***
|
|
Self-rated Health
|
-0.1264
|
***
|
-0.0915
|
**
|
-0.5451
|
***
|
|
Depression
|
-0.0806
|
*
|
-0.1685
|
***
|
-0.0687
|
*
|
|
|
|
|
|
|
|
|
|
Help_total
|
Help_outside
|
Help_within
|
|
Chronic diseases
|
-0.0904
|
*
|
-0.0910
|
*
|
-0.1170
|
*
|
|
Self-rated Health
|
-0.0243
|
|
-0.0352
|
*
|
-0.3504
|
**
|
|
Depression
|
-0.0569
|
*
|
-0.0857
|
*
|
0.0025
|
|
|
|
Effects of health
variables
|
Effects of confounders
|
Reverse causality
issues
|
|
Help-giving Total
|
All coefficients on health variables,
which are of our main interest, are of the expected, negative sign and
significant; but only after controlling for reverse causality
|
Significant and of expected sign:
Gender, age, education, physical inactivity, memory, welfare regimes
|
Only with the inclusion of the
instruments for each health variable, are
the results as expected
|
|
Help-giving Outside
|
All coefficients on health variables,
which are of our main interest, are of the expected, negative sign and
significant; but only after controlling for reverse causality
|
Significant and of expected sign: Age,
education, household size, physical inactivity, memory, welfare regimes
|
Only with the inclusion of the
instruments for each health variable, are
the results as expected
|
|
Help-giving Within
|
All coefficients on health variables,
which are of our main interest, are of the expected, negative sign and
significant; but only after controlling for reverse causality and including
an auxiliary variable
|
Significant and of expected sign:
Gender, age, income, employment status, household size, physical inactivity,
memory, welfare regimes
|
One does not observe the expected
relationships even after endogeneity is provided for by the instrumental
variable correction. Only with the final intervention, inclusion of the
auxiliary variable of receiving is care within household the issue solved,
providing the (negative) sign and significance of almost all of the
coefficients on health variables.
|
|
|
|
Abstract
Informal care is a widespread and important segment of long-term care, which is carried out independently of or in parallel with formal care, i.e. as a complement or replacement. Informal caregivers represent the backbone of long-term care, as has been witnessed by numerous international studies. In our article we focus on the relationship between the health status of the respondent and the decision to provide informal help to others as well as the intensity of the care. We show that this relationship is endogenous (reverse causality), using different measures of health and instrumental variables from Wave 5 and Wave 3 of SHARE Survey, and determine the causal effects of health on informal care, provided within and/or outside household. We also model the effect of various different covariates on informal caregiving. In conclusion we provide reflections on the research and discuss the policy relevance of the study.
Keywords: informal care; caregivers; health; reverse causality; instrumental variables; SHARE
JEL: J14, I11, C31, C36
1 Introduction and literature review
The causal relationship between informal caregiving and (poor) health has been established in several studies (e.g. Schulz and Sherwood,  2008; Schulz and Beach, 2008; Schulz and Beach,  1999; Pinquart and Sörensen, 1999; Pinquart and Sörensen,  2003; Roth et al., 2003; Roth et al.,  2009; Vitaliano, Zhang and Scanlon, 2009; Vitaliano, Zhang and Scanlon,  2003). Yet, what still remained under-researched is the effect of health on informal caregiving. As we show in the article, the results of basic correlations using common datasets on ageing in Europe (like SHARE) often confirm the negative sign of the relationship: particularly for caregivers within a household, those with worse health tend to give help more often. The question that motivating this article therefore, is: what is driving this relationship. 2003). Yet, what still remained under-researched is the effect of health on informal caregiving. As we show in the article, the results of basic correlations using common datasets on ageing in Europe (like SHARE) often confirm the negative sign of the relationship: particularly for caregivers within a household, those with worse health tend to give help more often. The question that motivating this article therefore, is: what is driving this relationship.
As stated in Hlebec, Srakar and Majcen (  2017 2017), long term care is considered an emerging key issue in discussing the social inclusion or exclusion of the older population in modern European society (e.g. Theobald,  2005 2005; Motel-Klingebiel, Tesch-Roemer and von Kondratowitz,  2005 2005). Cross-national econometric studies of the relationship between formal and informal care for older adults in western European countries have become a booming field (Suanet, van Groenou and van Tilburg,  2012 2012).
Organizing care for older people is one of the most important issues in European countries which are characterized by a rise in the share of the elderly, which is caused by longer life expectancy and declining fertility rates. The share of the population aged 80 years and over, which is the most likely to need care, grew from 1.5% in 1960 to nearly 5% in 2010 in Europe as a whole, and is expected to rise to 11% by 2050 and 12% by 2060 (OECD,  2013 2013; The Ageing Report, 2015). The share of people aged 20-64 will decline substantially from 61% in 2013 to 51% by 2060 (ibid.). Thus, we can expect a big increase in the need for care on one hand, and a smaller number of potential informal carers on the other. Both trends are likely to place greater demands on formal care systems across Europe.
The majority of older people wish to age and receive care in their own homes (Cantor,  1979 1979; Iecovich,  2014 2014). In 2011, in OECD countries 8.7% of people aged 65+ received care in their own homes as against 4.1% in institutions (OECD,  2013 2013). For people living at home, care can be provided by different parts of informal social networks like family members, friends or neighbours (Cantor,  1979 1979; Wenger,  1994 1994; Allen, Goldscheider and Ciambrone,  1999 1999; Blomgren et al.,  2008 2008). Care can also be provided by formal care workers such as providers of health and social care or migrant care workers (Iecovich,  2010 2010; Walsh and O’Shea,  2010 2010; Shutes and Chiatti,  2012 2012; Stevens, Hussein and Manthorpe,  2012 2012; Williams,  2012 2012). Very often, older people combine care from different sources: private and public care, formal and informal care, informal care by spouses, children and other informal sources (Litwin and Attias-Donfut,  2009 2009; Gannon and Davin,  2010 2010).
The type of care older people use depends on their preferences and their individual and social contexts (Andersen and Newman,  2005 2005). Some people prefer only informal care (Cantor,  1979 1979; 1991) and seek care first from their partners and children, then other family members, friends and neighbours. Only in cases where no informal caregivers are available will they accept formal care, provided they can afford it financially and depending on the range of services provided by the community. Formal care, therefore, may compensate for a lack of informal care and complement informal care when needs grow (Chappell and Blandford,  1991 1991; Denton,  1997 1997).
Informal carers provide a vast amount of care to older people in Europe as shown by data from the European Quality of Life Survey. About 6.4% (Denmark) to 20.1% (Lithuania) of the adult population in Europe provides care to their elderly or disabled relatives at least once or twice a week. On average, these family members deliver 12.5 hours of care to dependent family members. Care is frequently provided by spouses or children, sometimes also by friends and neighbours (Cantor,  1979 1979; Stoller and Pugliesi,  1988 1988; Allen, Goldscheider and Ciambrone,  1999 1999; Barrett and Lynch,  1999 1999). Most European countries support informal carers with specific policy measures (Mestheneos and Triantafillou,  2005 2005; Saraceno and Keck,  2010 2010; Colombo et al.,  2011 2011). Support for informal carers encompasses a variety of services in cash and in kind, services specified for working carers and others (e.g. a carer’s allowance, an allowance for the person being cared for, tax credits, additional benefits, paid leave, unpaid leave, flexible work arrangements, training/education, respite care, counselling).
There is a lot of literature (primary and meta-analysis) on the impacts of informal caregiving on caregivers’ health (e.g. Roth et al.,  2013 2013; Hiel et al.,  2015 2015; Vlachantoni,  2013 2013; Schulz and Sherwood,  2008 2008; Pinquart and Sorensen,  2003 2003;  2006 2006;  2007 2007). Interdisciplinary research has provided different research designs, sampling procedures, statistical methods of a heterogeneous nature. Health has been studied as psychological health and physical health (separately or simultaneously). Meta-analyses and other systematic reviews typically conclude that caregivers are more likely to experience depressive symptoms and have poorer physical health outcomes when compared with various samples of non-caregivers (Pinquart and Sörensen,  2003 2003; Schulz and Sherwood,  2008 2008; Vitaliano, Zhang and Scanlon,  2003 2003). Recent review (Bauer and Sousa-Poza,  2015 2015) pointed out that caregiving tends to lower the quality of the caregiver’s psychological health, which also has a negative impact on physical health outcomes. Some studies (Schoenmakers, van Tilburg and Fokkema,  2015 2015; Bauer and Sousa-Poza,  2015 2015) noted that: (a) literature reviewed is very heterogeneous – minimally comparable; (b) most studies are cross-sectional and thus do not/cannot account for endogeneity; (c) research often omits important controls (e.g. pre-existing illness).
However, insufficient attention has been paid to estimating and explaining the (reverse) causal relationship between health and caregiving, i.e. the effects of health on the provision of caregiving. The aim of the article is to explain this relationship in detail, including the heterogeneous behaviour across different types of care provision (within or outside a household).
In a recent article, Kaschowitz and Brandt (  2017 2017) provided a longitudinal analysis of the health effects of informal caregiving across Europe. Using data from the Survey of Health, Ageing and Retirement (SHARE, waves 1, 2, 3 and 5) and from the English Longitudinal Study of Ageing (ELSA, waves 2-5) they examined the connection between informal caregiving and self-perceived as well as mental health in a country=comparative perspective. They were able to show distinct differences in the relationship between reported health and the provision of informal care depending on whether individuals give care to someone inside or outside the household. Caregivers inside the household reported worse, while caregivers from outside the household reported better, health than non-caregivers. Their explanation is largely related to selection into caregiving: according to their findings, people in worse health take up care inside while people in better health take up care outside the household. Their results also show that the health consequences of caregiving vary not only between different welfare regimes but also among countries of similar welfare state types.
Based on the above, in our article we test three main hypotheses: H1: Older people in better health tend to provide more help to others 1. H2: The relationship between informal caregiving and health is of an endogenous, reverse causal nature. H3: There are significant differences in the relationship of health and informal caregiving or help-giving 2 within and outside a household 3.
The main method we use to verify the above hypotheses is regression analysis, using instrumental variables models to appropriately model the assumed reverse causality in the relationships studied.
The article is structured in the following way. In the next section, we will present basic considerations about the data and method used. In the third section, we will present the main results and robustness tests. In the final section, we will conclude with reflections on the research findings and policy implications.
2 Data and method
We use dataset derived from Wave 5 of the SHARE survey4. The Survey of Health, Ageing and Retirement in Europe (SHARE) is a multidisciplinary and crossnational panel database of micro data on health, socio-economic status and social and family networks of approximately 123,000 individuals (more than 293,000 interviews) from 20 European countries (+Israel) aged 50 or older5. SHARE is centrally coordinated by the Munich Centre for the Economics of Aging (MEA), the Max Planck Institute for Social Law and Social Policy. It is harmonized with the U.S. Health and Retirement Study (HRS) and the English Longitudinal Study of Ageing (ELSA) and has become a model for several ageing surveys worldwide. In the analysis, we also use data from Wave 3, SHARELIFE, which provides dana on life-histories of the respondents.
SHARE data collection is based on computer-assisted personal interviewing (CAPI). Exceptions are the drop off and vignette questionnaires, which are conducted via paper & pencil as well as the end-of-life interviews that can be conducted via CATI (computer-assisted telephone interview), too. The SHARE study is subject to continuous ethics review. During Waves 1 to 4, SHARE was reviewed and approved by the Ethics Committee of the University of Mannheim. Wave 4 and the continuation of the project were reviewed and approved by the Ethics Council of the Max Planck Society. In addition, the country implementations of SHARE were reviewed and approved by the respective ethics committees or institutional review boards whenever this was required (Börsch-Supan and Jürges,  2005 2005).
After including instruments from SHARE Wave 3, our final sample consists of 14,564 respondents from 11 European countries (Austria, Germany, Sweden, Netherlands, Spain, Italy, France, Denmark, Switzerland, Belgium, Czech Republic).
We include three main help-giving variables: Help-giving_out: binary variable for providing help outside a household. Help-giving_wtin: binary variable for providing help within a household. Helpgiving_tot: joined variable of Help-giving_out and Help-giving_wtin 6.
Graph 1 presents the distribution of the three variables over the countries and welfare regimes. We can see that the countries with the highest percentage of total help-giving and help-giving outside household are the Social Democratic/Scandinavian countries. They are followed by continental countries and some Eastern European ones, while, in particular, Mediterranean countries and Israel fall quite behind. Interestingly, those are the countries that, on the other hand, have the largest percentages of help-giving within a household.
Graph 1Distribution of the help-giving variables (%) DISPLAY Graph
Table 1 provides the actual quantities of people in the population providing help. Most of the relationships observed in graph 1 can be seen here as well, in particular the large number of people providing help within the household in Mediterranean countries.
Table 1Estimation of total help-givers, Deville-Särndal’s procedure DISPLAY Table
The main health variables we use in the analysis are: - Physical health: number of chronic diseases (dummy: 1 if a respondent has two or more chronic diseases; and 0 otherwise).
- Mental health: depression (dummy: 1 if a respondent has a score of 4 or more on the Euro-D Depression scale; and 0 otherwise).
- Subjective assessment of health: self-rated health status (dummy: 1 if less than very good; and 0 otherwise).
As control variables we use: - Gender: gender of the respondent, 0 for male, 1 for female.
- Age: age of the respondent in years.
- Education: education of the respondent in years of his/her schooling period.
- Income: nominal household income (variable thinc2 from the generated SHARE variables), winsorised to prevent the impact of outliers and transformed into tertiles (by country).
- Employment status: categorical variables, describing whether the respondent is employed, retired or in any other status (e.g. unemployed).
- Household size: size of the household of the respondent.
- Physical inactivity: binary variable, defined as never or almost never engaging in either moderate or vigorous physical activity.
- Memory: number of words, recalled after reading a list of ten words7.
- Welfare regimes: classification of the country of the respondent, based on Esping-Andersen (
 1990), into four types: 1 – continental (Austria, Germany, Netherlands, France, Switzerland, Belgium, Luxembourg); 2 – social democratic (Sweden, Denmark); 3 – Mediterranean (Spain, Italy); 4 – Eastern European (Czech Republic, Slovenia, Estonia). 1990), into four types: 1 – continental (Austria, Germany, Netherlands, France, Switzerland, Belgium, Luxembourg); 2 – social democratic (Sweden, Denmark); 3 – Mediterranean (Spain, Italy); 4 – Eastern European (Czech Republic, Slovenia, Estonia).
We also use the following auxiliary variable: - Receiving help: 1 if the respondent is receiving informal care within the household and 0 otherwise.
As instruments we use the following variables, all from Wave 3 of SHARE – SHARELIFE: - As instrument for the number of chronic diseases: sl_hs006: “childhood health: in hospital for 1 month+”.
- As instrument for mental health (depression): sl_hs009d3: “childhood illness 2: emotional, nervous, or psychiatric problem”.
- As instrument for self-rated health: sl_hs003_: childhood health status.
All instruments satisfy the two instrumental variable restrictions (see e.g. Wooldridge,  2010 2010), the second and the third are also very strong.
Instrumental variable (IV) estimation faces three perils of its own (Murray,  2006 2006): - IV estimation is inconsistent if the instruments are correlated with the disturbance term. This is the problem of “bad” or “invalid” instruments.
- IV estimation suffers persistent biases and size-of-test biases in even very large samples if the instruments used are only weakly correlated with explanatory variables responsible for bias in an OLS estimation. This is the problem of “weak” instruments.
- Interpreting the economic meaning of IV estimates can become problematic if the slope coefficients in one’s model are heterogeneous across observations. This is the problem of “ugly” instruments.
In our case, we face the problem of “ugly” instruments (this was confirmed by initial modellings not presented here) and to derive the proper results we have to model help-giving within and outside a household separately to model the heterogeneity in the model appropriately.
The main formal model we use is instrumental variables probit which fits models with dichotomous dependent variables and endogenous regressors. Formally, the model can be stated as: | y*1i = y2iβ + x1iγ + ui | (1 ) ) |
| y2i = x1i Π1 + x2i Π2 + vi | (2 ) ) |
We do not observe y*1i, instead, we observe 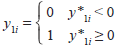 | (3 ) ) |
Graph 2 provides the basic picture we want to explore. It provides the distribution of health variables for those that provide help in total, outside and within a household. We can clearly see that for all three health variables, the providers of help in total and outside a household face lower problems with health, while those within a household face even higher health problems. This is a puzzle we will solve and provide an explanation for in our analysis.
Graph 2Distribution of the main three health variables (left: number of chronic diseases; middle: self-rated health; right: EURO-Depression scale), based on help-giving within and outside the household and total help-giving DISPLAY Graph
3 Results and robustness checks
Table 2 shows the results when using the “ordinary” econometric models with no endogeneity provided for (all models all of probit variety). Interestingly and surprisingly, it is apparent that the more health problems there are (i.e. the more chronic diseases, worse self-rated health and more depression symptoms) the greater the provision of help to others.
What is driving these results? This is of course the main research question of the article, elaborated in the introductory section. An apparent possibility is consideration of the reverse causality in the model. The supposed and basic causality structure imposes health as influencing informal caregiving. Yet, as we noted at the start when reviewing the evidence from the literature, informal caregiving can have (adverse) effects on health indicators as well.
To properly provide for this observation, we include instrumental variables for each of the three health variables. We instrument for number of chronic diseases by childhood health (whether the respondent was in a hospital for 1 month or more during his/her childhood); for mental health by having an emotional, nervous, or psychiatric problem in childhood; and for self-rated health by childhood health status.
Table 2Results of the models with no endogeneity provided for DISPLAY Table
Furthermore, as is shown on the right side of graph 3, we also need an additional intervention in the case of caregiving within a household. We need to include an additional, auxiliary variable for “receiving care” within a household, as we assume that care within a household is mutual (see e.g. Kaschowitz and Brandt,  2017 2017) and, therefore, it is likely that the health conditions of the members of the same household are connected with each other. The final causality structure is shown in graph 3 – at the left is the causal structure for help-giving in total and outside a household, where only reverse causality is present, while on the right is the causal structure for help-giving within a household, where beside reverse causality an auxiliary variable of receiving care within a household also needs to be included to provide consistent results.
As it turns out, all the models work very well when taking into account endogeneity and causal problems. Firstly, in table 3, we provide results for total help-giving where it is apparent that with the inclusion of the instrument (the endogeneity tests confirm the presence of reverse causality in all cases) all coefficients on health variables, which are of our main interest, are now of the expected, negative sign and significant.
Graph 3Modelling of reverse causality in the model DISPLAY Graph
Table 3Results of models, endogeneity controlled for, total help-giving DISPLAY Table
Also in table 4, we show the results for help-giving outside a household. Here, the significance of the relationship becomes even stronger, confirming the problem of the ugly instrument we have been discussing previously. All the other considerations (signs and significance of the coefficients on main and control variables) from table 3 are almost the same.
Table 4Results of models, endogeneity controlled for, help-giving outside a household DISPLAY Table
Finally, table 5 presents the results for the modelling of help-giving within a household. Here, one does not observe the expected relationships even after the endogeneity is provided for by the instrumental variable correction. On the other hand, the final intervention, inclusion of the auxiliary variable of receiving care within household finally solves the issue and provides the (negative) sign and significance of all of the coefficients (except for depression, where the coefficient is not statistically significant) which is in accordance with the expectations and our hypotheses.
Table 5Results of models, endogeneity controlled for, help-giving within household DISPLAY Table
In table 6, we provide results of several robustness checks to verify our main findings. Firstly, we exclude the additional health variables (physical inactivity, memory) which influence the provision of help-giving but could be related also to our three main health variables. The results do not change in any manner – indeed, the coefficient becomes of even stronger significance.
Secondly, we restrict the age of the respondents to 65+ 8. Once again, there are no changes, furthermore, now even the coefficient on depression for the help-giving within a household becomes significant and of the expected sign.
Finally, we include an additional instrument (presence of formal care) to control for possible reverse causality between providing and receiving help within household. Again, no significant changes can be observed in the main relationship under study.
Table 6 Results of robustness tests, top: exclusion of additional health variables due to additional endogeneity problems; middle: restricting the age of the respondents: 65+, bottom: including an additional instrument to control for reverse causality between providing and receiving help within a household DISPLAY Table
4 Conclusion
In conclusion, let’s firstly summarize the findings by the set of initial three hypotheses and present the main results of the paper. The latter are summarized in table 7.
Table 7Summarized main results of the paper by type of help-giving DISPLAY Table
H1: Older people in better health tend to provide more help to others.
The hypothesis is clearly confirmed. In all three cases we were able to confirm it and provide strong reasoning for the somewhat strange results that could be observed by basic descriptive statistics and basic econometric modellings not taking into account the specific causal relationships in the model. Indeed, the solution to this problem is the main contribution of the article and an important resource for future research in this area. It contributes significantly to the previous findings in e.g. Kaschowitz and Brandt (  2017 2017) and relates to the recent analysis in Calvó-Perxas et al. (  2018 2018).
H2: Relationship between informal caregiving and health is of an endogenous, reverse causal nature.
We confirm the hypothesis on the basis of the testing as reported in tables 3, 4 and 5. All the tests confirmed the expected reverse causality, which is in line with the findings of the literature, standing for the presence of the negative effects of helpgiving on the health of the provider. As noted in the introductory section of our article, it is widely accepted that caregiving has an impact on caregivers’ health (Zarit, Reever and Bach-Peterson,  1980 1980; Hiel et al.,  2015 2015), and most caregivers have to deal with their own chronic illnesses as well (Jowsey et al.,  2013 2013; Stacey et al.,  2016 2016). Support measures are thus necessary to keep caregivers in good health, to maintain their quality of life, and to keep costs down, so that the informal caregiving system is maintained (Kaschowitz and Brandt,  2017 2017; Verbakel et al.,  2017 2017).
H3: There are significant differences in the relationship of health and informal caregiving between help-giving within and outside a household.
We confirm the hypothesis, which is clearly demonstrated by the descriptive statistics visualized in graph 2. Furthermore, we manage to provide an econometric/ causal solution that is able to explain the difference and control for it when modelling for our main relationship between health and informal help-giving. The findings strongly relate to the recent analysis of Calvó-Perxas et al. (  2018 2018) which finds that “the poorest health was reported by those giving care inside their households, which may be due to the fact of being emotionally closer to the recipient of care and to the fact that they cannot evade the care situation easily as those giving care outside their household” (Calvó-Perxas,  2018 2018).
The link to theory, presented in the initial section of the article, seems strong. We were able to connect the relationship of health and caregiving to theoretical expectations, but demonstrated that the usual positive link is to be found only after some econometric corrections and additional controlling variables. Also, we were able to confirm the findings of Kaschowitz and Brandt (  2017 2017) about the heterogeneity in the provision of care, with care provided within and outside a household having very opposite characteristics. Based on our findings, one would be tempted to ask for this heterogeneity in the provision of care to be explored to an even greater extent and in more detail, to find and explain the distinctions using, e.g. latent class modelling or cluster analysis of any other type.
Limitations of the analysis relate to the sample used, methods and theoretical background. In terms of the sample, the analysis is based on a cross section and should be extended in future also to a dynamic context. Also, constraints on respondents included could be imposed, related to their health and social condition. Also, the dataset allows us only to include help to a family member living outside one’s own household, a friend or neighbour. This should be extended also to people the respondent does not know, although SHARE does not allow such an extension. In terms of methods, other causal inference methods like directed acyclic graphs (possibly, using Bayesian networks), structural equation modelling and even mediation analysis could be used. If put in a dynamic context, more consistent causal analysis could be performed, using difference-and-differences, changes-in-changes and similar methods. Also, heterogeneity in the results could be analysed using latent class methods, quantile methods or cluster analysis. Finally, in terms of theoretical background and variables used, it could be interesting to extend the analysis to other health characteristics, linking the results also to limitations of daily life (ADL, IADL, GALI or functional limitations) or similar indicators.
The scientific contributions of the paper are clear. On the one hand, the article provides what seems to be a conclusive explanation for some “puzzles” in the data, observed previously by, e.g. Kaschowitz and Brandt (  2017 2017). The explanation is novel in particular for the help-giving provided within a household and is supported by some recent findings of Calvó-Perxas et al. (  2018 2018). Secondly, we provide some novel instruments to control reverse causality where health variables are included, based on Wave 3, i.e. the retrospective life histories of respondents. Finally, we provide a reflection on the policy recommendations to support the help-giving measures being implemented in many European countries.
There are some important pathways for future research. Firstly, improvements in the instrumental variable models used could be made, using additional variables, including social and material deprivation, relationship to the person receiving help, frequency of the help provided (some of this has been tried and the results are, again, very robust). We also confirm that Wave 3 of SHARE is a rich and interesting source for the construction of instrumental variables, something confirmed by the literature in the field. Possibly, additional instruments based on Wave 5 (the cross section used) could be tried and tested as well. It would also be interesting to model more deeply which is the more important predictor of informal caregiving: physical, mental or self-rated health? According to our results, physical health performed the best, but this question remains to be studied in future research. Finally, it would be interesting to model also the longitudinal aspects of the studied relationship and explore if it is dependent upon the contextual variables in the country studied.
Regarding the practical and policy recommendations, adopting measures to stimulate the health of potential and actual caregivers would tend to raise the level of help provided significantly, which was proven by our analysis. Although the finding might sound trivial, we observed that it could lead to absurd (opposite) conclusions if observed only by basic descriptive statistics or correlations. To this end, it was important to provide an explanation which is novel in the literature and differs quite significantly from the previous explanations, found, e.g. in Kaschowitz and Brandt (  2017 2017). In policy terms, measures used to stimulate health would contribute to the welfare of caregivers and by this to a better system of (informal) long term care which should be the desire of all. The question remaining for study here is how the effect we observed and studied is distributed among the studied population and whether it significantly differs not just by the type of provided help (outside or within a household) but also by some other characteristic of the respondent, the care receiver or context/country under study.
Funding
No special financial support for the article has been received.
Notes
* We would like to thank the two anonymous referees for valuable comments and suggestions.
1 All of those hypotheses relate to decision of providing care and not to quality or type of care.
2 In the article, we use the terms caregiving and help-giving as synonymous.
3 The studies also report a noticeable difference in respondents’ answers about the type of help received from other people (e.g. personal care vs. practical household help, see Hoefman, Meulenkamp and de Jong,  2017). In providing care within the household, assistance is related to personal care. Help-giving outside a household refers to personal care and practical care. 2017). In providing care within the household, assistance is related to personal care. Help-giving outside a household refers to personal care and practical care.
4 This paper uses data from SHARE Wave 5, see Börsch-Supan et al. ( 2013) for methodological details. The SHARE data collection has been primarily funded by the European Commission through FP5 (QLK6-CT-2001-00360), FP6 (SHARE-I3: RII-CT-2006-062193, COMPARE: CIT5-CT-2005-028857, SHARELIFE: CIT4-CT-2006-028812) and FP7 (SHARE-PREP: N°211909, SHARELEAP: N°227822, SHARE M4: N°261982). Additional funding from the German Ministry of Education and Research, the U.S. National Institute on Aging (U01_AG09740-13S2, P01_AG005842, P01_AG08291, P30_AG12815, R21_AG025169, Y1-AG-4553-01, IAG_BSR06-11, OGHA_0 2013) for methodological details. The SHARE data collection has been primarily funded by the European Commission through FP5 (QLK6-CT-2001-00360), FP6 (SHARE-I3: RII-CT-2006-062193, COMPARE: CIT5-CT-2005-028857, SHARELIFE: CIT4-CT-2006-028812) and FP7 (SHARE-PREP: N°211909, SHARELEAP: N°227822, SHARE M4: N°261982). Additional funding from the German Ministry of Education and Research, the U.S. National Institute on Aging (U01_AG09740-13S2, P01_AG005842, P01_AG08291, P30_AG12815, R21_AG025169, Y1-AG-4553-01, IAG_BSR06-11, OGHA_0
5 For more details, see Börsch-Supan et al.,  2013; 2013;  2015; Malter and Börsch-Supan, 2015; Malter and Börsch-Supan,  2015; Börsch-Supan, 2015; Börsch-Supan,  2016. 2016.
6 For the explanation of the two variables, see descriptions above.
7 In SHARE, there is also the variable of delayed recall of words which is not used here – but robustness checks have been done using this variable as a control as well with no significant changes in the results.
8 An additional check for the group of 80+ has been done with no changes in results.
* We would like to thank the two anonymous referees for valuable comments and suggestions.
1 All of those hypotheses relate to decision of providing care and not to quality or type of care.
2 In the article, we use the terms caregiving and help-giving as synonymous.
3 The studies also report a noticeable difference in respondents’ answers about the type of help received from other people (e.g. personal care vs. practical household help, see Hoefman, Meulenkamp and de Jong,  2017 2017). In providing care within the household, assistance is related to personal care. Help-giving outside a household refers to personal care and practical care.
4 This paper uses data from SHARE Wave 5, see Börsch-Supan et al. (  2013 2013) for methodological details. The SHARE data collection has been primarily funded by the European Commission through FP5 (QLK6-CT-2001-00360), FP6 (SHARE-I3: RII-CT-2006-062193, COMPARE: CIT5-CT-2005-028857, SHARELIFE: CIT4-CT-2006-028812) and FP7 (SHARE-PREP: N°211909, SHARELEAP: N°227822, SHARE M4: N°261982). Additional funding from the German Ministry of Education and Research, the U.S. National Institute on Aging (U01_AG09740-13S2, P01_AG005842, P01_AG08291, P30_AG12815, R21_AG025169, Y1-AG-4553-01, IAG_BSR06-11, OGHA_0
5 For more details, see Börsch-Supan et al.,  2013 2013;  2015 2015; Malter and Börsch-Supan,  2015 2015; Börsch-Supan,  2016 2016.
6 For the explanation of the two variables, see descriptions above.
7 In SHARE, there is also the variable of delayed recall of words which is not used here – but robustness checks have been done using this variable as a control as well with no significant changes in the results.
8 An additional check for the group of 80+ has been done with no changes in results.
Disclosure statement
The authors declare there is no conflict in interest related to this article.
References
Allen, S. M., Goldscheider, F. and Ciambrone, D. A., 1999. Gender Roles, Marital Intimacy, and Nomination of Spouse as Primary Caregiver. The Gerontologist, 39(2), pp. 150–158 [ CrossRef]
Andersen, R. and Newman, J. F., 2005. Societal and Individual Determinants of Medical Care Utilization in the United States. The Milbank Quarterly, 83(4) [ CrossRef]
Barrett, A. E. and Lynch, S. M., 1999. Caregiving Networks of Elderly Persons: Variation by Marital Status. The Gerontologist, 39(6), pp. 695–704 [ CrossRef]
Bauer, J. M. and Sousa-Poza, A., 2015. Impacts of Informal Caregiving on Caregiver Employment. Health and Family. IZA.
Blomgren, J. [et al.], 2008. Determinants of home-based formal help in community-dwelling older people in Finland. European Journal of Ageing, 5(4), pp. 335–347 [ CrossRef]
Börsch-Supan, A. [et al.] (eds.), 2015. Ageing in Europe - Supporting Policies for an Inclusive Society. Berlin: De Gruyter[ CrossRef]
Börsch-Supan, A. [et al.], 2013. Data Resource Profile: The Survey of Health, Ageing and Retirement in Europe (SHARE). International Journal of Epidemiology, 42(4), pp. 992–1001 [ CrossRef]
Börsch-Supan, A. and Jürges, H. (eds.), 2005. The Survey of Health, Ageing and Retirement in Europe – Methodology. Mannheim: MEA, Max Planck Institute for Social Law and Social Policy.
Börsch-Supan, A., 2016. Survey of Health, Ageing and Retirement in Europe (SHARE) Wave 5. Release version: 5.0.0. SHARE-ERIC. Data set [ CrossRef]
Calvó-Perxas, L. [et al.], 2018. What seems to matter in public policy and the health of informal caregivers? A cross-sectional study in 12 European countries. PLoS ONE, 13(3): e0194232 [ CrossRef]
Cantor, M. H., 1979. Neighbors and friends An overlooked resource in the informal support system. Research on Aging, 1(4), pp. 434–463 [ CrossRef]
Cantor, M. H., 1991. Family and community: Changing roles in an aging society. The Gerontologist, 31(3), pp. 337–346 [ CrossRef]
Chappell, N. and Blandford, A., 1991. Informal and formal care: exploring the complementarity. Ageing and Society, 11(3), pp. 299–317 [ CrossRef]
Colombo, F. [et al.], 2011. OECD Health Policy Studies Help Wanted? Providing and Paying for Long-Term Care: Providing and Paying for Long-Term Care. Paris: OECD.
Denton, M., 1997. The linkages between informal and formal care of the elderly. Canadian Journal on Aging, 16(1), pp. 30–50 [ CrossRef]
Esping-Andersen, G., 1990. Three worlds of welfare capitalism. Cambridge: Polity Press.
Gannon, B. and Davin, B., 2010. Use of formal and informal care services among older people in Ireland and France. The European Journal of Health Economics, 11(5), pp. 499–511 [ CrossRef]
Hiel, L. [et al.], 2015. Providing personal informal care to older European adults: should we care about the caregivers’ health? Preventive Medicine, 70, pp. 64–68 [ CrossRef]
Hlebec, V., Srakar, A. and Majcen, B., 2017. LTC determinants of care arrangements for older people in Europe: evidence from SHARE. Presented at the 3rd Transforming care conference "Innovation and sustainability", Milan, June 26, 2017.
Hoefman, R. J., Meulenkamp, T. M. and De Jong, J. D., 2017. Who is responsible for providing care? Investigating the role of care tasks and past experiences in a cross-sectional survey in the Netherlands. BMC Health Services Research, 17, pp. 477 [ CrossRef]
Iecovich, E., 2010. Tasks performed by primary caregivers and migrant live-in homecare workers in Israel. International Journal of Ageing & Later Life, 5(2), pp. 53–75 [ CrossRef]
Jowsey, T. [et al.], 2013. Time to care? Health of informal older carers and time spent on health related activities: an Australian survey. BMC Public Health, 22(13), pp. 374 [ CrossRef]
Kaschowitz, J. and Brandt, M., 2017. Health effects of informal caregiving across Europe: A longitudinal approach. Soc Sci Med, 173, pp. 72–80 [ CrossRef]
Litwin, H. and Attias-Donfut, C., 2009. The inter-relationship between formal and informal care: a study in France and Israel. Ageing & Society, 29(1), pp. 71–91 [ CrossRef]
Malter, F. and Börsch-Supan, A. (eds.), 2015. SHARE Wave 5: Innovations & Methodology. Munich: MEA, Max Planck Institute for Social Law and Social Policy.
Mestheneos, E. and Triantafillou, J., 2005. Supporting Family Carers of Older People in Europe-The Pan-European Background Report (Vol. 1). Siglo del Hombre Editores.
Motel-Klingebiel, A., Tesch-Roemer, C. and Von Kondratowitz, H.-J., 2005. Welfare states do not crowd out the family: evidence for mixed responsibility from comparative analyses. Ageing & Society, 25(6), pp. 863–882 [ CrossRef]
Murray, M. P., 2006. Avoiding Invalid Instruments and Coping with Weak Instruments. Journal of Economic Perspectives, 20(4), pp. 111–132 [ CrossRef]
OECD. 2013. Health at a Glance 2013: OECD Indicators. Paris: OECD [ CrossRef]
Pinquart, M. and Sörensen, S., 2003. Differences between caregivers and noncaregivers in psychological health and physical health: A meta-analysis. Psychology and Aging, 18(2), pp. 250–267 [ CrossRef]
Pinquart, M. and Sörensen, S., 2006. Gender differences in caregiver stressors, social resources, and health: An updated meta-analysis. Journals of Gerontology. Series B, Psychological Sciences and Social Sciences, 61(1), pp. 33–45 [ CrossRef]
Pinquart, M. and Sörensen, S., 2007. Correlates of physical health of informal caregivers: A metaanalysis. Journals of Gerontology. Series B, Psychological Sciences and Social Sciences, 62(2), pp. 126–137 [ CrossRef]
Roth, D. L. [et al.], 2009. Family caregiving and emotional strain-associations with quality of life in a large national sample of middle-aged and older adults. QualLife Res, 18(6), pp. 679–688 [ javascript:nicTemp();CrossRef]
Roth, D. L. [et al.], 2013. Family caregiving and all-cause mortality: Findings from a population-based propensity-matched analysis. American Journal of Epidemiology, 178, pp. 1571–1578 [ CrossRef]
Saraceno, C. and Keck, W., 2010. Can We Identify Intergenerational Policy Regimes in Europe? European Societies, 12(5), pp. 675–696 [ CrossRef]
Schoenmakers, E. C., Van Tilburg, T. G. and Fokkema, T., 2015. Problem-focused and emotion-focused coping options and loneliness: How are they related? European Journal of Ageing, 12, pp. 153–161 [ CrossRef]
Schulz, R. and Beach, S., 1999. Caregiving as a risk factor for mortality. Journal of the American Medical, 282(23), pp. 2215–2219 [ CrossRef]
Schulz, R. and Sherwood, P., 2008. Physical and mental health effects of family caregiving. American Journal of Nursing, 108 (9-Supplement), pp. 23–27 [ CrossRef]
Shutes, I. and Chiatti, C., 2012. Migrant labour and the marketisation of care for older people: The employment of migrant care workers by families and service providers. Journal of European Social Policy, 22(4), pp. 392–405 [ CrossRef]
Stacey, A. F. [et al.], 2016. Unpaid Informal Caregivers in South Australia: Population Characteristics, Prevalence and Age-Period-Cohort Effects 1994–2014. PLoS One, 20(11), p. 9 [ CrossRef]
Stevens, M., Hussein, S. and Manthorpe, J., 2012. Experiences of racism and discrimination among migrant care workers in England: Findings from a mixed-methods research project. Ethnic and Racial Studies, 35(2), pp. 259–280 [ CrossRef]
Stoller, E. P. and Pugliesi, K. L., 1988. Informal Networks of Community-Based Elderly Changes in Composition over Time. Research on Aging, 10(4), pp. 499–516 [ CrossRef]
Suanet, B., Van Groenou, M. B. and Van Tilburg, T., 2012. Informal and formal home-care use among older adults in Europe: can cross-national differences be explained by societal context and composition? Ageing & Society, 32(3), pp. 491–515 [ CrossRef]
Theobald, H., 2005. Social exclusion and care for the elderly. Theoretical concepts and changing realities in European welfare states. WZB Discussion Paper, No. 301. Berlin: WZB.
Verbakel, E. [et al], 2017. Informal care in Europe: findings from the European Social Survey (2014) special module on the social determinants of health. Eur J Public Health, 1 (27, suppl_1), pp. 90–95 [ CrossRef]
Vitaliano, P., Zhang, J. and Scanlan, J. M., 2003. Is caregiving hazardous to one’s physical health? A meta-analysis. Psychological Bulletin, 129(6), pp. 946–972 [ CrossRef]
Vlachantoni, A. [et al], 2013. Informal care, health and mortality. Maturitas, 72(2), pp. 114–118 [ CrossRef]
Wenger, G. C., 1994. Support Networks of Older People: A Guide for Practitioners. Bangor: Centre for Social Policy Research & Development, University of Wales.
Williams, F., 2012. Converging variations in migrant care work in Europe. Journal of European Social Policy, 22(4), pp. 363–376 [ CrossRef]
Wooldridge, J. M., 2010. Econometric Analysis of Cross Section and Panel Data. Cambridge, MA: MIT Press.
Zarit, S. H., Reever, K. E. and Bach-Peterson, J., 1980. Relatives of the impaired elderly: correlates of feelings of burden. Gerontologist, 20(6), pp. 649–655 [ CrossRef]
Allen, S. M., Goldscheider, F. and Ciambrone, D. A., 1999. Gender Roles, Marital Intimacy, and Nomination of Spouse as Primary Caregiver. The Gerontologist, 39(2), pp. 150–158 [ CrossRef]
Andersen, R. and Newman, J. F., 2005. Societal and Individual Determinants of Medical Care Utilization in the United States. The Milbank Quarterly, 83(4) [ CrossRef]
Barrett, A. E. and Lynch, S. M., 1999. Caregiving Networks of Elderly Persons: Variation by Marital Status. The Gerontologist, 39(6), pp. 695–704 [ CrossRef]
Bauer, J. M. and Sousa-Poza, A., 2015. Impacts of Informal Caregiving on Caregiver Employment. Health and Family. IZA.
Blomgren, J. [et al.], 2008. Determinants of home-based formal help in community-dwelling older people in Finland. European Journal of Ageing, 5(4), pp. 335–347 [ CrossRef]
Börsch-Supan, A. [et al.] (eds.), 2015. Ageing in Europe - Supporting Policies for an Inclusive Society. Berlin: De Gruyter[ CrossRef]
Börsch-Supan, A. [et al.], 2013. Data Resource Profile: The Survey of Health, Ageing and Retirement in Europe (SHARE). International Journal of Epidemiology, 42(4), pp. 992–1001 [ CrossRef]
Börsch-Supan, A. and Jürges, H. (eds.), 2005. The Survey of Health, Ageing and Retirement in Europe – Methodology. Mannheim: MEA, Max Planck Institute for Social Law and Social Policy.
Börsch-Supan, A., 2016. Survey of Health, Ageing and Retirement in Europe (SHARE) Wave 5. Release version: 5.0.0. SHARE-ERIC. Data set [ CrossRef]
Calvó-Perxas, L. [et al.], 2018. What seems to matter in public policy and the health of informal caregivers? A cross-sectional study in 12 European countries. PLoS ONE, 13(3): e0194232 [ CrossRef]
Cantor, M. H., 1979. Neighbors and friends An overlooked resource in the informal support system. Research on Aging, 1(4), pp. 434–463 [ CrossRef]
Cantor, M. H., 1991. Family and community: Changing roles in an aging society. The Gerontologist, 31(3), pp. 337–346 [ CrossRef]
Chappell, N. and Blandford, A., 1991. Informal and formal care: exploring the complementarity. Ageing and Society, 11(3), pp. 299–317 [ CrossRef]
Colombo, F. [et al.], 2011. OECD Health Policy Studies Help Wanted? Providing and Paying for Long-Term Care: Providing and Paying for Long-Term Care. Paris: OECD.
Denton, M., 1997. The linkages between informal and formal care of the elderly. Canadian Journal on Aging, 16(1), pp. 30–50 [ CrossRef]
Esping-Andersen, G., 1990. Three worlds of welfare capitalism. Cambridge: Polity Press.
Gannon, B. and Davin, B., 2010. Use of formal and informal care services among older people in Ireland and France. The European Journal of Health Economics, 11(5), pp. 499–511 [ CrossRef]
Hiel, L. [et al.], 2015. Providing personal informal care to older European adults: should we care about the caregivers’ health? Preventive Medicine, 70, pp. 64–68 [ CrossRef]
Hlebec, V., Srakar, A. and Majcen, B., 2017. LTC determinants of care arrangements for older people in Europe: evidence from SHARE. Presented at the 3rd Transforming care conference "Innovation and sustainability", Milan, June 26, 2017.
Hoefman, R. J., Meulenkamp, T. M. and De Jong, J. D., 2017. Who is responsible for providing care? Investigating the role of care tasks and past experiences in a cross-sectional survey in the Netherlands. BMC Health Services Research, 17, pp. 477 [ CrossRef]
Iecovich, E., 2010. Tasks performed by primary caregivers and migrant live-in homecare workers in Israel. International Journal of Ageing & Later Life, 5(2), pp. 53–75 [ CrossRef]
Jowsey, T. [et al.], 2013. Time to care? Health of informal older carers and time spent on health related activities: an Australian survey. BMC Public Health, 22(13), pp. 374 [ CrossRef]
Kaschowitz, J. and Brandt, M., 2017. Health effects of informal caregiving across Europe: A longitudinal approach. Soc Sci Med, 173, pp. 72–80 [ CrossRef]
Litwin, H. and Attias-Donfut, C., 2009. The inter-relationship between formal and informal care: a study in France and Israel. Ageing & Society, 29(1), pp. 71–91 [ CrossRef]
Malter, F. and Börsch-Supan, A. (eds.), 2015. SHARE Wave 5: Innovations & Methodology. Munich: MEA, Max Planck Institute for Social Law and Social Policy.
Mestheneos, E. and Triantafillou, J., 2005. Supporting Family Carers of Older People in Europe-The Pan-European Background Report (Vol. 1). Siglo del Hombre Editores.
Motel-Klingebiel, A., Tesch-Roemer, C. and Von Kondratowitz, H.-J., 2005. Welfare states do not crowd out the family: evidence for mixed responsibility from comparative analyses. Ageing & Society, 25(6), pp. 863–882 [ CrossRef]
Murray, M. P., 2006. Avoiding Invalid Instruments and Coping with Weak Instruments. Journal of Economic Perspectives, 20(4), pp. 111–132 [ CrossRef]
OECD. 2013. Health at a Glance 2013: OECD Indicators. Paris: OECD [ CrossRef]
Pinquart, M. and Sörensen, S., 2003. Differences between caregivers and noncaregivers in psychological health and physical health: A meta-analysis. Psychology and Aging, 18(2), pp. 250–267 [ CrossRef]
Pinquart, M. and Sörensen, S., 2006. Gender differences in caregiver stressors, social resources, and health: An updated meta-analysis. Journals of Gerontology. Series B, Psychological Sciences and Social Sciences, 61(1), pp. 33–45 [ CrossRef]
Pinquart, M. and Sörensen, S., 2007. Correlates of physical health of informal caregivers: A metaanalysis. Journals of Gerontology. Series B, Psychological Sciences and Social Sciences, 62(2), pp. 126–137 [ CrossRef]
Roth, D. L. [et al.], 2009. Family caregiving and emotional strain-associations with quality of life in a large national sample of middle-aged and older adults. QualLife Res, 18(6), pp. 679–688 [ javascript:nicTemp();CrossRef]
Roth, D. L. [et al.], 2013. Family caregiving and all-cause mortality: Findings from a population-based propensity-matched analysis. American Journal of Epidemiology, 178, pp. 1571–1578 [ CrossRef]
Saraceno, C. and Keck, W., 2010. Can We Identify Intergenerational Policy Regimes in Europe? European Societies, 12(5), pp. 675–696 [ CrossRef]
Schoenmakers, E. C., Van Tilburg, T. G. and Fokkema, T., 2015. Problem-focused and emotion-focused coping options and loneliness: How are they related? European Journal of Ageing, 12, pp. 153–161 [ CrossRef]
Schulz, R. and Beach, S., 1999. Caregiving as a risk factor for mortality. Journal of the American Medical, 282(23), pp. 2215–2219 [ CrossRef]
Schulz, R. and Sherwood, P., 2008. Physical and mental health effects of family caregiving. American Journal of Nursing, 108 (9-Supplement), pp. 23–27 [ CrossRef]
Shutes, I. and Chiatti, C., 2012. Migrant labour and the marketisation of care for older people: The employment of migrant care workers by families and service providers. Journal of European Social Policy, 22(4), pp. 392–405 [ CrossRef]
Stacey, A. F. [et al.], 2016. Unpaid Informal Caregivers in South Australia: Population Characteristics, Prevalence and Age-Period-Cohort Effects 1994–2014. PLoS One, 20(11), p. 9 [ CrossRef]
Stevens, M., Hussein, S. and Manthorpe, J., 2012. Experiences of racism and discrimination among migrant care workers in England: Findings from a mixed-methods research project. Ethnic and Racial Studies, 35(2), pp. 259–280 [ CrossRef]
Stoller, E. P. and Pugliesi, K. L., 1988. Informal Networks of Community-Based Elderly Changes in Composition over Time. Research on Aging, 10(4), pp. 499–516 [ CrossRef]
Suanet, B., Van Groenou, M. B. and Van Tilburg, T., 2012. Informal and formal home-care use among older adults in Europe: can cross-national differences be explained by societal context and composition? Ageing & Society, 32(3), pp. 491–515 [ CrossRef]
Theobald, H., 2005. Social exclusion and care for the elderly. Theoretical concepts and changing realities in European welfare states. WZB Discussion Paper, No. 301. Berlin: WZB.
Verbakel, E. [et al], 2017. Informal care in Europe: findings from the European Social Survey (2014) special module on the social determinants of health. Eur J Public Health, 1 (27, suppl_1), pp. 90–95 [ CrossRef]
Vitaliano, P., Zhang, J. and Scanlan, J. M., 2003. Is caregiving hazardous to one’s physical health? A meta-analysis. Psychological Bulletin, 129(6), pp. 946–972 [ CrossRef]
Vlachantoni, A. [et al], 2013. Informal care, health and mortality. Maturitas, 72(2), pp. 114–118 [ CrossRef]
Wenger, G. C., 1994. Support Networks of Older People: A Guide for Practitioners. Bangor: Centre for Social Policy Research & Development, University of Wales.
Williams, F., 2012. Converging variations in migrant care work in Europe. Journal of European Social Policy, 22(4), pp. 363–376 [ CrossRef]
Wooldridge, J. M., 2010. Econometric Analysis of Cross Section and Panel Data. Cambridge, MA: MIT Press.
Zarit, S. H., Reever, K. E. and Bach-Peterson, J., 1980. Relatives of the impaired elderly: correlates of feelings of burden. Gerontologist, 20(6), pp. 649–655 [ CrossRef]
|
|
|
September, 2018
III/2018
|








 2008
2008